When should BiPAP be used

Christopher Lucas
Published Feb 15, 2026
Bilevel positive airway pressure (BiPAP) is a type of noninvasive ventilation. It is used when you have a condition that makes it hard to breathe like sleep apnea, COPD, asthma, heart conditions and other ailments.
When do you use CPAP vs BiPAP?
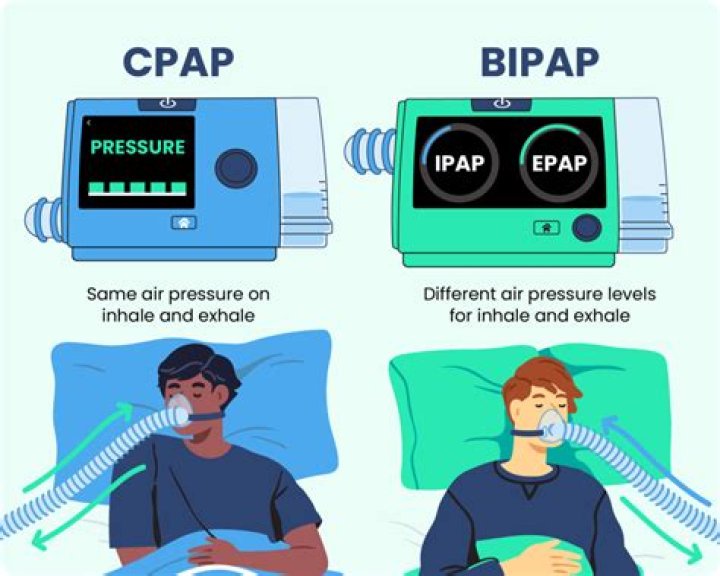
The CPAP machine is usually used to treat mild to moderate sleep apnea. But depending on the severity of sleep apnea, doctors may recommend a BiPAP machine instead. Patients requiring high levels of CPAP pressure are often more comfortable using BiPAP.
Is a BiPAP machine life support?
No. Removing BiPAP is a decision to stop a medical treatment and allow the underlying condition to take its natural course. Removal of BiPAP results in the person’s death, usually within hours. Medical assistance in dying, or MAID, is different.
What are the indications for CPAP and BiPAP?
NIV/CPAP indications COPD with respiratory acidosis (pH <7.35) Hypercapnic respiratory failure secondary to chest wall deformity (scoliosis, thoracoplasty) or neuromuscular disease. Weaning from tracheal intubation.Is BiPAP used for Covid?
Evidence suggests that bi-level positive airway pressure (BiPAP) support may be used in the hospital setting with appropriate precautions for intubated COVID-19 patients experiencing Acute Respiratory Distress Syndrome (ARDS).
Which is worse BiPAP or CPAP?
CPAPBiPAPTypical Pressure Range4 to 20 cm H2O4 to 25 cm H2O
Is BiPAP good for Covid?
NIV includes Continuous Positive Airway Pressure (CPAP) and Bi-Level Positive Airway Pressure (BiPAP). CPAP is the method of choice with the use of BiPAP for those with complex respiratory conditions who contract COVID-19.
Does BiPAP use oxygen?
BiPAP allow oxygen entry during expiratory phase during which pressure inside mask is low.Is BiPAP considered non invasive ventilation?
Bilevel positive airway pressure (BiPAP) is probably the most common mode noninvasive positive pressure ventilation and requires provisions for inspiratory positive airway pressure (IPAP) and expiratory positive airway pressure (EPAP).
How long can a patient be on BiPAP before needing intubation?BiPAP cannot be continued without a break for too long (>24-48 hours) without causing nutritional problems and pressure necrosis of the nasal skin. Thus, if the patient fails to improve on BiPAP for 1-2 days, then a transition to HFNC or intubation is needed.
Article first time published onIs BiPAP mechanical ventilation?
One type of non-invasive mechanical ventilation is called CPAP (continuous positive airway pressure) and another is called BiPAP (bi-level positive airway pressure). Invasive mechanical ventilation uses a machine to push air and oxygen into your lungs through a tube in your windpipe.
Is BiPAP good for pneumonia?
Conclusion. BiPAP ventilator airway pressure by face mask ventilation can reduce the rate of endotracheal intubation in the treatment of severe pneumonia caused by influenza A (H1N1) virus in acute respiratory failure. It could be an effective approach in the emergency treatment with clinical value.
Is BiPAP an intubation?
BiPAP may be used in the hospital setting with appropriate precautions for intubated COVID-19 patients experiencing Acute Respiratory Distress Syndrome (ARDS). Use of invasive BiPAP on an emergency basis may delay or obviate the need for mechanical ventilation in appropriate COVID-19 patients.
Are you intubated for BiPAP?
If a patient is not improving by this time, then endotracheal intubation should be considered. The indications for use of BiPAP are: Respiratory failure not requiring immediate intubation with: medically unacceptable or worsening alveolar hypoventilation.
How long can a person be on a ventilator in an ICU?
Some people may need to be on a ventilator for a few hours, while others may require one, two, or three weeks. If a person needs to be on a ventilator for a longer period of time, a tracheostomy may be required.
Does a BiPAP machine help COPD?
BiPAP machines provide two different levels of air pressure, which makes breathing out easier than it is with a CPAP machine. For this reason, BiPAP is preferred for people with COPD. It lessens the work it takes to breathe, which is important in people with COPD who expend a lot of energy breathing.
What is Covid pneumonia?
In the case of COVID pneumonia, the damage to the lungs is caused by the coronavirus that causes COVID-19. When COVID pneumonia develops, it causes additional symptoms, such as: Shortness of breath. Increased heart rate.
Can you use a nasal mask with BiPAP?
If you’ve been using a BiPAP to treat sleep apnea, you might be wondering why can’t find a mask made specifically for your BiPAP machine. Well, the answer is simple, all CPAP masks are technically BiPAP masks because they are designed to work with any CPAP or BiPAP machine.
What are the side effects of BiPAP?
- Slight skin irritation from wearing the face mask.
- Dry mouth and/or dry nasal passages.
- Stomach bloating from breathing in too much air.
- Allergy to the mask’s material, which can cause skin breakouts or respiratory issues.
Can a ventilator be used without intubation?
Non-invasive ventilation refers to ventilatory support without tracheal intubation. This can be used as a first step in patients who require some ventilatory support and who are not profoundly hypoxaemic.
Does BiPAP improve oxygenation?
While CPAP works to improve only oxygenation (hypoxemic respiratory failure), the use of BiPAP improves not only oxygenation but also ventilation with the use of pressure support. There are different types of BiPAP modes.
Is a breathing machine the same as a ventilator?
Your doctor might call it a “mechanical ventilator.” People also often refer to it as a “breathing machine” or “respirator.” Technically, a respirator is a mask that medical workers wear when they care for someone with a contagious illness. A ventilator is a bedside machine with tubes that connect to your airways.
Does BiPap require spontaneous breathing?
Bi-Level Positive Airway Pressure Ventilation (BIPAP) Hence, this method requires triggering and synchronization with the patient’s spontaneous breathing. Triggering the respiratory cycle is achieved by one of three modes: Spontaneous (S) (or assist).
What are the three modes of operation of BiPap machines?
- Spontaneous mode (S): In s mode all the breaths are patient triggered and cycled. …
- Spontaneous timed mode (S/TD): In S/TD mode breaths are patient triggered and machine trigerred, patient cycled and machine cycled.
Does BiPAP push fluid out of the lungs?
Studies show BiPAP is very helpful for CHF, supporting your breathing so you don’t have to work as hard to inhale. It also helps your heart. Some people might say that it pushes fluid out of your lungs, and though it might happen to a small degree, it’s not the main reason BiPAP is helpful for CHF.
Does BiPAP increase risk for aspiration?
BiPAP can provide greater oxygenation and ventilation support. However, BiPAP carries risks of mucus plugging, aspiration, and impaired patient monitoring.
Is high flow nasal cannula considered non-invasive ventilation?
High-flow nasal cannula (HFNC) oxygen therapy is a recent technique delivering a high flow of heated and humidified gas. HFNC is simpler to use and apply than noninvasive ventilation (NIV) and appears to be a good alternative treatment for hypoxemic acute respiratory failure (ARF).
What is a BiPAP machine in the hospital?
A BiPAP (Bi-level Positive Airway Pressure) machine is a non-invasive form of therapy that delivers pressurized air via a mask to the patient’s airways to assist in breathing.