What is oculomotor system

Emma Valentine
Published Feb 15, 2026
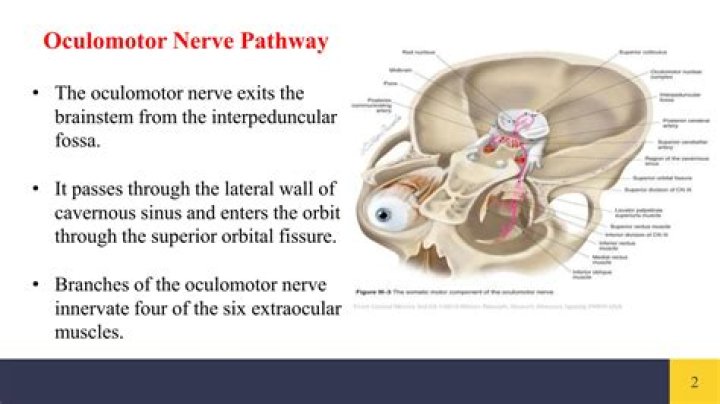
Definition. The oculomotor system consists of interconnected regions throughout the central nervous system that interact to control various eye movements. It includes different brainstem nuclei, the superior colliculus of the midbrain, and various regions throughout the cerebral cortex.
What is oculomotor behavior?
The oculomotor behaviors observed were task-specific, and their spatial and temporal patterns revealed a common strategy. Rather than memorizing a pattern and then replicating the pattern from memory, subjects made frequent eye movements, referring to the model pattern an average of more than 1.5 times per block.
What does ocular motor mean?
Ocular motor apraxia (OMA) is the absence of, or a defect in, the control of voluntary, purposeful eye movement. Children with this condition have difficulty moving their eyes in a desired direction. In other words, their saccades (the quick, simultaneous movement of both eyes in the same direction) are abnormal.
What are oculomotor disturbances?
Oculomotor disturbances or nystagmus—periodic, mostly involuntary, eye movements—are of topodiagnostic importance especially in patients with lesions in the brainstem region (which often means additional brainstem symptoms) or cerebellum.What function is associated with the oculomotor nerve?
The oculomotor nerve is the third cranial nerve (CN III). It allows movement of the eye muscles, constriction of the pupil, focusing the eyes and the position of the upper eyelid.
How is oculomotor diagnosed?
A comprehensive, binocular vision assessment is the only way to accurately identify and diagnose Oculomotor Dysfunction as well as other binocular vision deficits.
What are the different eye movements?
There are four basic types of eye movements: saccades, smooth pursuit movements, vergence movements, and vestibulo-ocular movements. … Saccades are rapid, ballistic movements of the eyes that abruptly change the point of fixation.
What is oculomotor apraxia?
Ataxia with oculomotor apraxia is a condition characterized by problems with movement that worsen over time. The hallmark of this condition is poor coordination and balance (ataxia), which is often the first symptom.What causes oculomotor dysfunction?
Oculomotor Dysfunction can be caused by slow or faulty development of muscle control, a central nervous disease or acquired/traumatic brain injury. This can easily be diagnosed during an eye exam. By 2 months of age, a child should be able to follow a moving object.
Is oculomotor apraxia progressive?Ataxia-oculomotor apraxia 4 The disorder is progressive, and most patients become wheelchair-bound in the second or third decade (summary by Bras et al., 2015).
Article first time published onWhich part of the brain controls eye movement?
In the frontal lobe, three main areas are involved in eye movement control [2]: the frontal eye field (FEF), the supplementary eye field (SEF) and the dorsolateral prefrontal cortex (DLPFC).
What muscle elevates the eyeball?
The first of these muscles, the superior rectus muscle, elevates the eye, allowing the eye to look up. The antagonist of the superior rectus muscle is the inferior rectus muscle, which depresses the eye, allowing the eye to look down.
What happens if the oculomotor nerve is damaged?
Damage to any of these nerves or the muscle or muscles they innervate causes dysconjugate gaze, which results in characteristic patterns of diplopia (double vision). In addition, with oculomotor nerve damage, patients also lose their pupillary constriction to light as well as the elevation of their eyelid.
What is oculomotor nerve palsy?
Oculomotor nerve palsy or oculomotor neuropathy is an eye condition resulting from damage to the third cranial nerve or a branch thereof.
How is the oculomotor nerve tested?
Step One: Open the right eyelid and shine the light into the right eye. Look only into the right eye to assess for a response. A normal response is a brisk constriction of the right pupil. If the pupil gets larger or has a sluggish response, it is considered abnormal.
Is eye movement voluntary or involuntary?
Eye movement includes the voluntary or involuntary movement of the eyes, helping in acquiring, fixating and tracking visual stimuli. A special type of eye movement, rapid eye movement, occurs during REM sleep. The eyes are the visual organs of the human body, and move using a system of six muscles.
What are the two main types of eye movements that direct our eyes from one location to another how are they different?
The binocular movements (the movements of the two eyes) fall into two classes, the conjugate movements, when both eyes move in the same direction, as in a change in the direction of gaze, and disjunctive movements, when the eyes move in opposite directions.
What is good eye movement?
The angle of eye movement was quantified using a modified limbus test. Results : The normal ranges of eye movement were 44.9±7.2° in adduction, 44.2±6.8° in adduction, 27.9±7.6° in elevation, and 47.1±8.0° in depression.
How many muscles control the movement of the eye?
For each eye, six muscles work together to control eye position and movement. Two extraocular muscles, the medial rectus and lateral rectus, work together to control horizontal eye movements (Figure 8.1, left). Contraction of the medial rectus pulls the eye towards the nose (adduction or medial movement).
Does convergence insufficiency go away?
Eye care providers can diagnose CI with a health history and eye exam. Most of the time, it will go away if you regularly do special eye exercises.
How do you treat saccadic eye movement?
Saccadic deficiencies can be treated using vision therapy at any age, and it can help to improve reading speed and ability. Some of the treatments that might be used are monocular exercises done with a patch including charts, games, hitting a Marsden Ball, and doing eye stretches and jumps.
How common is vertical Heterophoria?
It is believed that up to 10% of the general population suffers from vertical heterophoria (VH). VH can be congenital, meaning that it’s something you’re born with. It can also develop after a traumatic brain injury (TBI), even if it’s just a mild concussion.
Can convergence insufficiency get worse?
If untreated, CI can lead to more serious eye problems such as lazy eye (amblyopia) or even an eye turn (strabismus). If the convergence problems are left untreated, suppression can result.
How is ocular motor dysfunction treated?
Your eye muscles are just like other muscles in your body; exercising them can help them perform better. As a result, vision therapy is one of the best treatments for ocular motor dysfunction. Vision therapy allows you to practice new skills to strengthen eye muscles’ ability to work together effectively.
What is the difference between apraxia and aphasia?
There are, though, distinct differences between the two. Aphasia describes a problem in a person’s ability to understand or use words in and of themselves. This may make it hard for someone with the condition to speak, read, or write. But apraxia does not describe a problem with language comprehension.
Is ocular motor dysfunction hereditary?
Cogan type ocular motor apraxia is a genetic condition for which the inheritance pattern has not been well established. It is not clear if it is inherited as an autosomal recessive genetic trait or an autosomal dominant genetic trait.
What's the difference between ataxia and apraxia?
In marked gait or postural ataxia, patients cannot stand with the feet together and the eyes open. Gait apraxia is a motor planning deficit and, thus, has a cerebral localization. Patients with gait apraxia have a hard time getting started with walking and may have a “magnetic” or shuffling gait.
What part of the brain causes apraxia?
Apraxia is caused by a defect in the brain pathways that contain memory of learned patterns of movement. The lesion may be the result of certain metabolic, neurological or other disorders that involve the brain, particularly the frontal lobe (inferior parietal lobule) of the left hemisphere of the brain.
What is AOA1?
Ataxia with oculomotor apraxia type 1 (AOA1) is characterized by childhood onset of slowly progressive cerebellar ataxia, followed by oculomotor apraxia and a severe primary motor peripheral axonal motor neuropathy.
What causes Ideomotor apraxia?
Cause. The most common cause of ideomotor apraxia is a unilateral ischemic lesion to the brain, which is damage to one hemisphere of the brain due to a disruption of the blood supply, as in a stroke. There are a variety of brain areas where lesions have been correlated to ideomotor apraxia.
Which part of the brain controls visual reflexes and eye movements?
tectum: The dorsal part of the midbrain, responsible for auditory and visual reflexes. tegmentum: The ventral portion of the midbrain, a multisynaptic network of neurons involved in many unconscious homeostatic and reflexive pathways.