What is dental periapical

Christopher Lucas
Published Feb 16, 2026
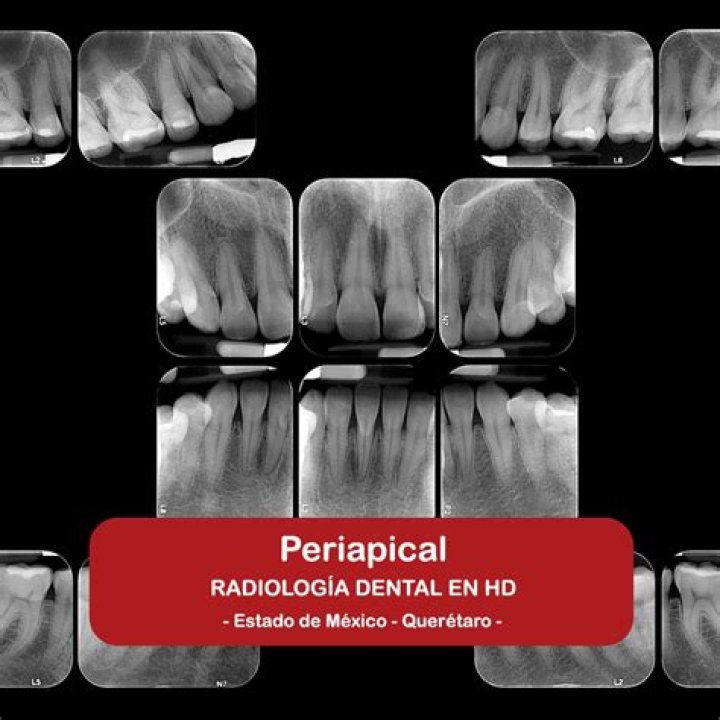
Periapical X-rays show the whole tooth — from the crown, to beyond the root where the tooth attaches into the jaw. Each periapical X-ray shows all teeth in one portion of either the upper or lower jaw. Periapical X-rays detect any unusual changes in the root and surrounding bone structures.
What is a periapical technique?
Periapical radiography is a commonly used intraoral imaging technique in radiology and may be a component of your radiologic examination. Periapical radiographs provide important information about the teeth and surrounding bone.
What is periapical film?
A periapical x-ray or “PA film” will show one or two teeth in their entirety in one single image, right from the crown of the tooth which is the part exposed in the mouth to the very tips of the tooth roots located in the jawbone, as well as the surrounding bone supporting this tooth.
What is a periapical examination?
Introduction. Periapical radiographs are the most common intraoral radiographic images produced in the examination of the oral and maxillofacial structures. They provide important information about the teeth and surrounding structures, including the alveolar processes, periodontium and neighbouring anatomic structures.What causes a periapical lesion?
In contrast, the primary cause of periapical lesions is endodontic infection. PAMPs-triggered immune response induces proinflammatory cytokines and subsequent periapical pathosis, including chronic inflammation and bone destruction. The primary cause of periapical lesions does not overlap with metabolic disorders.
What are the three types of dental images?
There are three types of diagnostic radiographs taken in today’s dental offices — periapical (also known as intraoral or wall-mounted), panoramic, and cephalometric. Periapical radiographs are probably the most familiar, with images of a few teeth at a time captured on small film cards inserted in the mouth.
What is a periapical Radiolucency?
Periapical radiolucency is the descriptive term for radiographic changes which are most often due to apical periodontitis and radicular cysts, that is, inflammatory bone lesions around the apex of the tooth which develop if bacteria are spread from the oral cavity through a caries-affected tooth with necrotic dental …
What is a vitality test in dentistry?
There are two major types of dental pulp tests. “Vitality testing” assesses the blood supply to the tooth, whilst “sensitivity testing” tests the sensory supply.How do you take periapical digital radiography?
In the case of periapical radiographs, the digital receptor should be placed parallel to the full length of the crown and root of the teeth being imaged. To achieve the best placement and patient comfort, the digital receptor should be placed closer to the midline rather than close to the teeth.
What is palpation in dentistry?Palpation. The dentist will be able to check the sensitivity of the gums around the tooth by palpating, or gently massaging the gums over the roots of the tooth or teeth suspected of causing your pain. They will also palpate control teeth, or those that are not suspected of causing pain, as a comparison.
Article first time published onWhy does dentist use cold test?
In practical application, cold testing, more than any other single test, allows the clinician to “zero in” on the source of the pulpal inflammation and/or confirm the diagnosis of a necrotic pulp.
What is a periapical disease?
Periapical periodontitis or apical periodontitis (AP) is an acute or chronic inflammatory lesion around the apex of a tooth root, most commonly caused by bacterial invasion of the pulp of the tooth.
How are periapical lesions treated?
The treatment modalities for periapical lesions include non-surgical root canal treatment, periapical surgery, or tooth extraction. If non-surgical treatment is deemed ineffective or difficult, periapical surgery is the treatment of choice.
What is the main cause of periodontal disease?
Periodontal (gum) disease is an infection of the tissues that hold your teeth in place. It’s typically caused by poor brushing and flossing habits that allow plaque—a sticky film of bacteria—to build up on the teeth and harden.
What does Endo mean in dentistry?
“Endo” is the Greek word for “inside” and “odont” is Greek for “tooth.” Endodontic treatment, or root canal treatment, treats the soft pulp tissue inside the tooth. An endodontist is a dentist who specializes in saving teeth.
Why is it called Phoenix abscess?
A phoenix abscess is an acute exacerbation of a chronic periapical lesion. It is a dental abscess that can occur immediately following root canal treatment. Another cause is due to untreated necrotic pulp (chronic apical periodontitis). It is also the result of inadequate debridement during the endodontic procedure.
What is the difference between periodontal abscess and periapical abscess?
It is a type of dental abscess. A periodontal abscess occurs alongside a tooth, and is different from the more common periapical abscess, which represents the spread of infection from a dead tooth (i.e. which has undergone pulpal necrosis). To reflect this, sometimes the term “lateral (periodontal) abscess” is used.
What is occlusal xray?
Occlusal. These X-rays show the roof or floor of the mouth. They are used to find extra teeth, teeth that have not yet broken through the gums, jaw fractures, a cleft in the roof of the mouth (cleft palate), cysts, abscesses, or growths.
What is 3D xray?
Unlike 2D x-rays, three-dimensional x-ray imaging was developed to help create an understanding of the entire mouth by designing a 3D rendition of the oral cavity. The 3D image captures a true 3d image of the mouth and allows the dentist to study the mouth in slices, similar to a CT scan.
What is root canal of teeth?
A root canal is a dental procedure involving the removal of the soft center of the tooth, the pulp. The pulp is made up of nerves, connective tissue, and blood vessels that help the tooth grow. In the majority of cases, a general dentist or endodontist will perform a root canal while you’re under local anesthesia.
What are the techniques for periapical radiography?
There are two types of techniques used for periapical radiographs: bisecting angle, and paralleling. The bisecting technique may have to be used for patients unable to accommodate the film positioning device used in the paralleling technique. These patients may include adults with low palatal vaults and children.
What is labial mounting?
Technique: Current convention is that all dental radiographs are mounted/interpreted with “labial mounting”. This means that the film is viewed from the outside in. … If you are interpreting a standard radiograph, the key to properly identifying the imaged side is the embossed dot, which is on one corner of the film.
What is the preferred method to get a good periapical image?
The paralleling technique is considered to be the best way to take periapical X-rays and when used correctly, it should produce reliable images with minimal distortion.
When is a periapical radiograph indicated?
Periapical/occlusal radiographs are indicated for identifying or confirming pathology, evaluating dental development, dento-alveolar trauma, deep carious lesions, periapical pathology, and oral involvement of systemic disease.
When do you need a cavity test?
If employed, the cavity test is initiated on a suspicious tooth, without anesthetic, and involves drilling a small window through either enamel or a restoration to dentin. The cavity test will stimulate a vital pulp and provoke a painful response when dentin is invaded.
What is endodontic diagnosis?
In order to render proper treatment, a complete endodontic diagnosis must include both a pulpal and a periapical diagnosis for each tooth evaluated. Examination and Diagnostic Procedures. Endodontic diagnosis is similar to a jigsaw puzzle—diagnosis cannot be made from a single isolated piece of information (4).
How do I check my teeth vitality?
Pulp tests, such as electric pulp testing and thermal tests, involve methods used to determine the vitality of the pulp. Periapical tests include percussion and palpation. While these tests do not provide information about the pulp, they indicate whether there is inflammation in the periapical tissues.
What is tooth Pericoronitis?
Pericoronitis is swelling and infection of the gum tissue around the wisdom teeth, the third and final set of molars that usually appear in your late teens or early 20s. It is most common around the lower wisdom teeth.
What is pulp cap indirect?
An indirect pulp cap is a procedure that protects a compromised tooth without exposed pulp. It may help you avoid more invasive procedures like tooth extraction or a root canal. It retains the tooth and allows its roots to continue developing.
What is control tooth?
Anytime you are testing a tooth, you need to have “control” teeth. Choose teeth adjacent to or across the arch from the tooth in question. **Always start your testing on the control teeth. Be gentle. Give clear instructions to your patient to avoid having to re-test a tooth and causing more discomfort for your patient.
Why do dentist hit your teeth?
It’s important to treat a dying or dead tooth as soon as possible. That’s because left untreated, the bacteria from the dead tooth can spread and lead to the loss of additional teeth. It could also affect your jawbone and gums. Your dentist may treat a dead or dying tooth with a procedure known as a root canal.