What are sterile techniques

Christopher Lucas
Published May 05, 2026
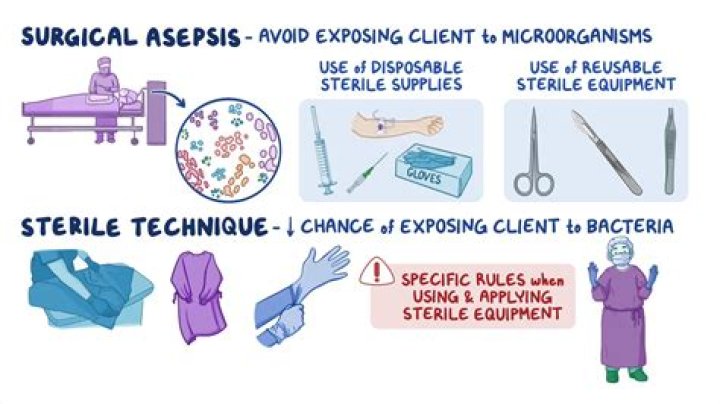
Sterile technique means practicing specific procedures before and during invasive procedures to help prevent SSIs and other infections acquired in hospitals, ambulatory surgery centers, physicians’ offices, and all other areas where patients undergo invasive procedures.
What is sterile technique example?
Aseptic techniques range from simple practices, such as using alcohol to sterilize the skin, to full surgical asepsis, which involves the use of sterile gowns, gloves, and masks. Healthcare professionals use aseptic technique practices in hospitals, surgery rooms, outpatient care clinics, and other healthcare settings.
What does sterile mean in microbiology?
What is the Definition of Sterile? Sterile conditions require the complete absence of microorganisms including bacteria, fungus, and their spores. For cleanroom applications, that means that a 70% IPA solution doesn’t kill bacterial or fungal spores, and therefore not an effective sterilant.
What are the sterile techniques in biotechnology?
Aseptic techniques are a large set of practices that prevent contamination by eliminating the unintentional transfer of microorganisms and cells. In general, these practices involve a combination of environmental control, personal hygiene, and sterilizing equipment and media.What is considered sterile?
Sterile means free from germs. When you care for your catheter or surgery wound, you need to take steps to avoid spreading germs. Some cleaning and care procedures need to be done in a sterile way so that you do not get an infection. Follow your health care provider’s instructions on using sterile technique.
Why is sterile technique important give two reasons?
a technique for isolating pure cultures by spreading organisms on an agar plate. Why is sterile technique important? This technique is important because it prevents contamination of your culture with organisms from the environment and to prevent the culture from contaminating you or others.
Why is sterile technique used?
Sterile technique. The strictest form of aseptic technique, sterile technique is intended to provide a space that has no germs whatsoever. Sterile technique is used in surgeries and other large, invasive procedures where infection could be the most dangerous.
Which is one of the sterility technique?
Sterile technique may include the use of sterile equipment, sterile gowns, and gloves (Perry et al., 2014). Sterile technique is essential to help prevent surgical site infections (SSI), an unintended and oftentimes preventable complication arising from surgery.What is the difference between sterile and aseptic technique?
In the context of medicine, aseptic and sterile both mean germ-free. Aseptic is most commonly applied in the context of techniques and procedures, while sterile is most commonly used to describe environments and instruments that have been cleaned (sterilized). Sterile also means “incapable of producing offspring.”
Why is sterile technique important in microbiology?Sterile technique is ESSENTIAL when working with microorganisms! It is important to protect strains from contamination with other strains and from the many undefined microbes in the environment.
Article first time published onWhat is the sterile technique in labs?
Aseptic technique refers to a set of routine procedures done to prevent sterile solutions and cultures from becoming contaminated by unwanted microorganisms in the laboratory.
What is the importance of sterile technique in preparing culture media?
Using the proper aseptic technique can significantly reduce/minimize the risk of contamination. Aseptic technique commonly maintains pure stock cultures and single spore culture while transferring cultures into fresh media.
What is another name for sterile technique?
Asepsis refers to any procedure that is performed under sterile conditions. This includes medical and laboratory techniques (such as with bacterial cultures). There are two types of asepsis – medical and surgical.
What are 3 types of sterilization?
- Plasma Gas Sterilizers. …
- Autoclaves. …
- Vaporized Hydrogen Peroxide Sterilizers.
What does sterile mean in biology?
incapable of producing offspring; not producing offspring. barren; not producing vegetation: sterile soil. Botany. noting a plant in which reproductive structures fail to develop. bearing no stamens or pistils.
What is the process of sterilization?
Sterilization describes a process that destroys or eliminates all forms of microbial life and is carried out in health-care facilities by physical or chemical methods. … Disinfection describes a process that eliminates many or all pathogenic microorganisms, except bacterial spores, on inanimate objects (Tables 1 and 2).
What are 4 common aseptic techniques?
According to The Joint Commission, there are four chief aspects of the aseptic technique: barriers, patient equipment and preparation, environmental controls, and contact guidelines. Each plays an important role in infection prevention during a medical procedure.
How do you maintain a sterile field?
- Disinfect any work surfaces and allow to them thoroughly dry before placing any sterile supplies on the surface.
- Be aware of areas of sterile fields that are considered contaminated:
Why are aseptic techniques used in the lab?
In the microbiology lab we use aseptic technique to: Prevent contamination of the specific microorganism we are working with. Prevent contamination of the room and personnel with the microorganism we are working with.
What is aseptic area?
An aseptic area is a premise in a clean area, designed, constructed, serviced and used with an intention to prevent the microbial contamination of the product.
Why is sterility important in experiments concerning bacteria and other microbes?
Researchers employ several sterile techniques to avoid contamination. Sterile technique is used to attempt to eliminate as much contamination as possible from all laboratory settings. Hands, equipment, and work surfaces must be sterile, or free of living organisms, to avoid contamination.
What is a sterile environment in tissue culture?
Sterile Environments for Plant Tissue Culturing Plant tissue culture in a controlled environment drastically reduces pathogens, fungi, and other microbes that interfere with reproductive mechanisms. Sterile conditions require the complete absence of microorganisms including bacteria, fungi, yeast, and their spores.
How do you create a sterile environment?
A sterile field is an area created by placing sterile surgical drapes around the patient’s surgical site and on the stand that will hold sterile instruments and other items needed during surgery.
What is difference between sterile and sterilization?
While sterile means the complete absence of bacteria, viruses, and fungi along with spores, it doesn’t distinguish between specific pathogens. … A sterilization technique aims to rid an environment of all living microorganisms.
What is sterile and non-sterile?
Sterile compounding is used when there is a high risk of infection, such as drugs given as an injection, through an IV, or directly into the eyes. … Non-sterile compounding medications include pills, liquids, gels, lotions, ointments, creams, shampoos, lip balms, and more.
What is a sterile object?
Sterile persons or sterile objects may only contact sterile areas; non-sterile persons or items contact only non-sterile areas. The front of the sterile gown is sterile between the shoulders and the waist, and from the sleeves to two inches below the elbow. Non-sterile items should not cross over the sterile field.
What are sterility indicators sterile technique quiz?
What are sterility indicators? A strip placed inside the package that changes when exposed to high temperature. … This procedure requires her to prepare a sterile tray and put on sterile gloves.
What does non sterile mean?
Difference between Sterile and Non-sterile These packages can be non-sterile meaning that they are not free from germs or microorganisms. Sterile kits accede to the strictest of standards and regulations about infection control techniques to decrease the risks of contamination with bacteria and harmful organisms.
Why is it important to keep cultures sterile?
A sterile field is required for all invasive procedures to prevent the transfer of microorganisms and reduce the potential for surgical site infections.
What does it mean to maintain a sterile field and why is this important to have during surgery?
Maintaining a sterile field is an important component of infection prevention. These set of practices that are performed before, during and after invasive procedures reduce the number of potentially infectious microbes and help to reduce the risk of post procedure infection.
How do you sterilize culture media?
Media containing agar should be heated to dissolve the agar before autoclaving. Bring the medium to the boil without scorching or burning. Most culture media will require final sterilization in an autoclave at 121°C for 20 minutes.