Is pneumoperitoneum fatal

Christopher Lucas
Published Feb 16, 2026
Although tension pneumoperitoneum is a life-threatening condition, it is reversible if prompt diagnosis and immediate decompression are performed.
Is pneumoperitoneum a medical emergency?
Pneumoperitoneum is a medical emergency, which is defined as the presence of free air within the peritoneal cavity.
Is pneumoperitoneum require immediate surgery?
Pneumoperitoneum (best assessed on a cross-table or left lateral decubitus position) or presence of intra-abdominal fluid is a serious sign indicating a need for immediate surgical intervention.
Is pneumoperitoneum normal?
A pneumoperitoneum is common after abdominal surgery; it usually resolves 3-6 days after surgery, although it may persist for as long as 24 days after surgery. The peritoneum is a thin, serous membrane that lines the abdominal cavity.Is pneumoperitoneum painful?
Pneumoperitoneum in the presence of acute abdominal pain is well recognised as an indication for laparotomy. We present a case of acute abdominal pain in the presence of an incidental pneumoperitoneum secondary to the rupture of pneumatosis intestinalis.
How long does pneumoperitoneum last after laparoscopy?
Conclusions: We conclude that the residual pneumoperitoneum following laparoscopic surgery resolves within 3 days in 81% of patients and within 7 days in 96% of patients. The resolution time was significantly less in patients sustaining intraoperative bile spillage during cholecystectomy.
How do you develop pneumoperitoneum?
To establish the pneumoperitoneum, access to the peritoneal cavity can be gained through minilaparotomy and insertion of a laparoscopic trocar or Hasson trocar. Alternatively, an optical trocar can be blindly inserted into the peritoneal cavity, or a Verres needle may be inserted through the abdominal midline.
What is the surgery for pneumoperitoneum?
Laparoscopic surgery involves insufflation of a gas (usually carbon dioxide) into the peritoneal cavity producing a pneumoperitoneum. This causes an increase in intra-abdominal pressure (IAP). Carbon dioxide is insufflated into the peritoneal cavity at a rate of 4–6 litre min−1 to a pressure of 10–20 mm Hg.What is treatment for pneumoperitoneum?
Needle decompression is the immediate treatment of choice, followed by surgery in most cases. The authors report a case of TP that was managed at their medical center.
How long does postoperative pneumoperitoneum last?In most instances postoperative PP resolves within a week, but there are reported cases of PP lasting as long as 10–24 days [5–10]. In order to prevent negative laparotomies it is important to differentiate the post-operative delayed PP from ‘surgical PP’.
Article first time published onIs pneumoperitoneum normal after surgery?
A postoperative pneumoperitoneum (PP) following recent abdominal surgery may be a normal finding due to the air introduced during surgery or postoperative drains. However, a pneumoperitoneum on plain radiographs may also be an indicator of anastomotic leakage or gastrointestinal perforation [1-4].
How is pneumoperitoneum measured?
Pneumoperitoneum is achieved by insufflating carbon dioxide into the peritoneal cavity until a preset pressure is reached. During insufflation, both the pressure and total insufflated volume are measured.
What causes gas in the diaphragm?
Introduction: The most common cause of gas under diaphragm is hollow viscous perforation. In 10% of cases it can be due to rare causes, both abdominal and extra-abdominal, one of them being intra abdominal infection by gas forming organisms.
What causes air bubbles in abdomen?
Gas in the digestive tract comes from two sources: Aerophagia (air swallowing). This is usually caused by eating or drinking rapidly, chewing gum, smoking, or wearing loose dentures. Belching is the way most swallowed air leaves the stomach.
What is the cupola of diaphragm?
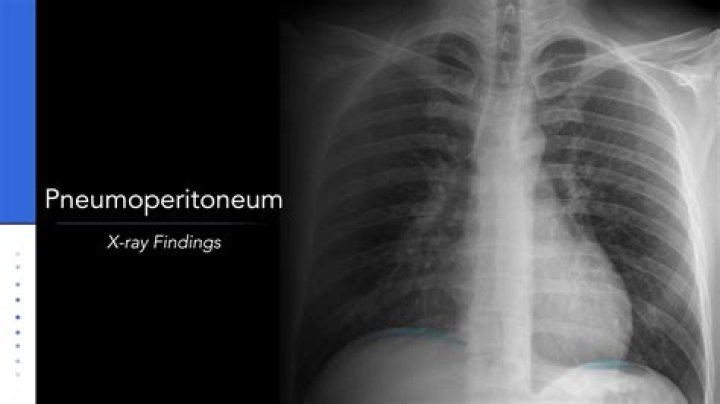
Cupola sign is seen on a supine chest or abdominal radiograph in the presence of pneumoperitoneum. It refers to dependent air that rises within the abdominal cavity of the supine patient to accumulate underneath the central tendon of the diaphragm in the midline.
Is pneumoperitoneum a diagnosis?
Pneumoperitoneum. Pneumoperitoneum due to perforated viscus is an emergent diagnosis that requires immediate surgical consultation and intervention. US is a useful tool that can be done at the bedside to rapidly make the diagnosis. Both low- and high-frequency transducers may be used to detect intraperitoneal free air.
Can you see pneumoperitoneum on ultrasound?
Pneumoperitoneum can be seen on ultrasound by two clear signs: The air within the peritoneal space rises and causes an enhanced peritoneal stripe sign (EPSS)– not to be confused with E-Point Septal Separation (EPSS) for left ventricular ejection fraction estimation.
Can pneumoperitoneum cause peritonitis?
Pneumoperitoneum refers to presence of free air within the peritoneal cavity, “Pneumoperitoneum induced Peritonitis” is synonymous of surgical pneumoperitoneum, as the leak of air and visceral contents contaminates the peritoneal cavity, producing peritonitis which mandates surgery.
How do you place trocars?
The anterior abdominal wall must be adequately elevated by hand, and the trocar is inserted directly into the cavity, aiming toward the pelvic hollow. As an alternative, the abdominal wall is elevated by pulling on two towel clips placed 3 cm on both sides of the umbilicus, and the trocar is inserted at a 90° angle.
What is Palmer's point?
Palmer’s point is described as the area in the left upper quadrant 3 cm below the costal margin and in the midclavicular line. Raoul Palmer MD was a French gynecologist many feel developed modern laparoscopy. 1n 1974 he described Palmer’s Point. This entry is utilized when midline adhesions are suspected.
Who is Hasson technique?
The open technique was first described by Hasson in 1970. This technique consists of creating a small umbilical incision under direct visualization to enter the abdominal cavity followed by the introduction of a blunt trocar. Pneumoperitoneum is then rapidly created.
Why do shoulders hurt after laparoscopy?
One type of pain that is unique to laparoscopy is the post laparoscopy shoulder pain due to the phrenic nerve irritation to the diaphragm caused by the CO2 gas that remains in the abdomen at the end of the procedure. When the patient sits up, the gas moves upwards to the diaphragm and irritates the shoulder.
How much pain is normal after laparoscopy?
After surgery, it’s normal to have a sore belly, cramping, or pain around the cuts the doctor made (incisions) for up to 4 days. You can expect to feel better and stronger each day. But you might get tired quickly and need pain medicine for a few days.
How does the gas from laparoscopic get out?
The procedure During laparoscopy, the surgeon makes a small cut (incision) of around 1 to 1.5cm (0.4 to 0.6 inches), usually near your belly button. A tube is inserted through the incision, and carbon dioxide gas is pumped through the tube to inflate your tummy (abdomen).
How do you treat free air in your stomach?
Treatment of PSI depends on the underlying cause, so that include elemental diet, antibiotics, steroids, hyperbaric oxygen therapy and surgery. In asymptomatic patients with free-air at X-ray and abdominal CT reporting gastrointestinal perforation direction, is a great handicap for the surgeon.
What is exploratory laparotomy surgery?
Exploratory laparotomy is an abdominal surgery that doctors sometimes use to diagnose abdominal issues. It is usually recommended when other testing did not diagnose or fully resolve an issue. Reasons to perform this surgery include: Abdominal trauma (for example, from an accident) Unexplained bleeding.
What is a peritoneal cavity?
Listen to pronunciation. (PAYR-ih-toh-NEE-ul KA-vuh-tee) The space within the abdomen that contains the intestines, the stomach, and the liver. It is bound by thin membranes.
How does pneumoperitoneum affect cardiovascular function?
In general, pneumoperitoneum in excess of 15mmHg has deleterious effects on the cardiovascular system. The pneu- moperitoneum compresses the vena cava and thus decreases venous return to the heart; this results in blood pooling in the lower half of the body and a decrease in cardiac output.
What are the risks of laparoscopic surgery?
The most common risks associated with laparoscopy are bleeding, infection, and damage to organs in your abdomen. However, these are rare occurrences. After your procedure, it’s important to watch for any signs of infection.
Why do they use co2 in surgery?
Carbon dioxide is used as an insufflation gas and as a cryotherapy agent. Carbon dioxide is commonly used as an insufflation gas for minimal invasive surgery (laparoscopy, endoscopy, and arthroscopy) to enlarge and stabilize body cavities to provide better visibility of the surgical area.
How do you get rid of shoulder pain after gallbladder surgery?
Other methods investigated to reduce shoulder tip pain include surgery with low-pressure insufflation, prewarmed gas, preemptive anti-inflammatory medication, preemptive diaphragmatic local anesthetic irrigation, postoperative drains, and subdiaphragmatic suction.