Is keratoconus noticeable

Emily Dawson
Published Feb 19, 2026
Keratoconus is not usually visible to the naked eye until the later stages of the disease. In severe cases, the cone shape is visible to an observer when the patient looks down while the upper lid is lifted.
How do I know if I have keratoconus?
- An abrupt change in vision.
- Seeing triple or double ghost images.
- Feeling uncomfortable driving at night because of blurry vision.
- Streaking lights.
- Objects far away as well as near appear to be distorted.
- A sudden change in vision in one eye.
Can an optometrist tell if you have keratoconus?
Optometrists can also play a large role in the diagnosis and treatment of keratoconus. Optometrists may diagnose keratoconus in their own office, or they may refer to other optometrists or ophthalmologists for additional diagnostic testing.
What does a person with keratoconus see?
Individuals with keratoconus often experience near-sightedness, blurry vision, distorted images, and extreme glare when viewing lights, especially at night. The condition is usually not painful, but can have a significant impact on an individual’s visual acuity.Can you go blind if you have keratoconus?
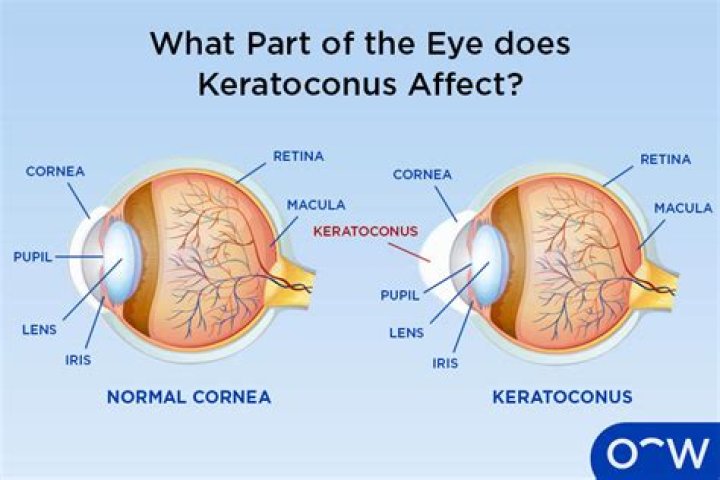
Keratoconus is a condition where the cornea becomes thin and stretched near its center, causing it to bulge forward into a conical shape. As a result vision becomes distorted. Keratoconus does not cause total blindness, however, without treatment it can lead to significant vision impairment.
How do you rule out keratoconus?
In order to make a diagnosis of keratoconus, the doctor must measure the curvature of the cornea. Several different tests can be performed to make the diagnosis. The test that is used most often is called topography. Topography measures the curvature of the surface of the eye and creates a colored “map” of the cornea.
Can I live a normal life with keratoconus?
The good news is that it does not have to be this way and that patients with keratoconus can go on to live normal lives just like any other person with good sight. You just need the proper treatment in order to get good vision back.
Can keratoconus stop progressing?
NEW YORK (Reuters Health) – Although keratoconus is often thought to stop progressing by the time patients are 30 to 40 years old, the corneal degeneration often continues beyond this point, according to researchers from New Zealand.Is keratoconus painful?
In rare cases, severe keratoconus causes a complication called corneal hydrops. This happens when part of your cornea breaks. This causes the fluid in your eye to flow into your cornea abnormally. This can cause severe pain and swelling.
Can keratoconus heal itself?Keratoconus does not fade on its own. The shape of your cornea can’t permanently change, even with medications, special contact lenses, or surgery. Remember, we have various options for reshaping your cornea, but keratoconus is a chronic, lifelong disorder. So don’t wait until things get worse.
Article first time published onCan I join the military with keratoconus?
According to Department of Defense Instruction on Medical Standards for Appointment, Enlistment, or Induction in the Military Services (DoDI 6130.03, Section 4c), people who have been diagnosed with keratoconus are not eligible to serve in the United States Armed Forces.
What is seeing halos around lights?
Seeing halos around lights is a result of diffraction, an effect that occurs when the light bends while entering the eye. Diffraction can sometimes be caused by glasses and contact lenses, but it can also be a disease’s side effect.
Can slit lamp examination detect keratoconus?
… corneal nerves on slit-lamp examination should prompt a search for other signs of keratoconus. Corneal ecta- sia is accompanied by thinning, which is generally greatest at the apex of the cone (Figures 1 and 3).
Does keratoconus affect both eyes?
Keratoconus usually affects both eyes, though it often affects one eye more than the other. It generally begins to affect people between the ages of 10 and 25. The condition may progress slowly for 10 years or longer.
Can keratoconus cause headaches?
Symptoms of Keratoconus are: Headaches and general eye pain: Both headaches and general eye pain can be attributed to Keratoconus. Eye irritation: excessive eye rubbing leading to eye irritation is a common symptom found in patients with Keratoconus.
Is keratoconus rare UK?
It is not generally considered an inherited disease, although rarely in some families more than one individual can be affected. Depending on ethnicity, keratoconus affects up to one in 450 people.
Is keratoconus easy to diagnose?
If your eye doctor says you have keratoconus, it’s possible that you’ve had it for years without knowing it. It’s difficult to detect this progressive eye disease affecting the cornea without a specific test.
Is cross linking worth it?
Although corneal crosslinking does come with a few limitations, eye surgeons and patients alike believe it is a worthwhile investment. Because corneal crosslinking works to lessen the bulging of the cornea, patients can wear contact lenses more comfortably following the procedure, making everyday life easier.
What can mimic keratoconus?
There are a variety of conditions that can resemble keratoconus including abnormal thinning and steepening of the outer (peripheral) edges of the cornea (pellucid marginal degeneration); thinning of the cornea and an abnormal globe-shaped (globular) or spherical form to the cornea (keratoglobus); chronic non-ulcerative …
What is mild keratoconus?
Mild Keratoconus = Lowest corneal thickness of ≥ 500μm. Moderate Keratoconus = Lowest corneal thickness of 300μm – 500μm. Advanced Keratoconus = Lowest corneal thickness of ≤ 300μm.
What is pentacam eye test?
It is a noncontact examination that photographs the surface of the eye. Pentacam is not a routine test. Rather, it is used in diagnosing certain types of problems, in evaluating a disease’s progression, in fitting some types of contact lenses, and in planning surgery.
What can worsen keratoconus?
Contact lenses that are not correctly fitted is another reason that Keratoconus gets worse. If the lenses are not accurately fitted on someone with Keratoconus, the lenses can rub against the diseased part of the cornea. The excessive rubbing causes symptoms to worsen by aggravating the already thin cornea.
Does Rubbing eyes cause keratoconus?
Several factors are affecting the development of keratoconus; eye-rubbing is the main factor which is causing a major number of eye injuries especially keratoconus. Eye rubbing causes the thinning of keratocyte, and the degree of effect of eye rubbing depends on the period and force of performing eye rubbing.
Does corneal cross-linking hurt?
Does the corneal cross-linking procedure hurt? No. The cross-linking procedure is painless. Anesthetic eye drops are used to avoid any discomfort during the procedure.
Do glasses help keratoconus?
Lenses. Eyeglasses or soft contact lenses. Glasses or soft contact lenses can correct blurry or distorted vision in early keratoconus. But people frequently need to change their prescription for eyeglasses or contacts as the shape of their corneas change.
How painful is corneal cross-linking?
Since the epithelium stays in place, most patients have little to no pain after their cross-linking procedure. But each person’s sensitivity varies, so you may have a little discomfort for the first few days.
How can I lower my keratoconus naturally?
Reversing Keratoconus But whatever the cause of your own Keratoconus, there is no way to naturally or medically reverse your Keratoconus with diet, exercise, drugs or other therapies.
Can dry eyes cause keratoconus?
Keratoconus can result in dry eyes because of your eyes inability to spread tears over your uneven cornea. Individuals with Keratoconus may experience dry eye naturally or as a byproduct of wearing contact lenses that further interfere with their eye’s ability to lubricate using tear drops.
What is the latest treatment for keratoconus?
Cross linking is one of the newest surgical keratoconus treatments. Cross linking for keratoconus was approved by the FDA in 2016. The UV light activated riboflavin greatly increases the connections between the collagen fibers (cross linking).
Can cross linking improve vision?
However, corneal collagen cross-linking – an advanced procedure approved by the U.S. Food and Drug Administration (FDA) in 2016 – can vastly improve vision in patients of all ages. Corneal collagen cross-linking (CXL) is not a cure for keratoconus, but it can help prevent the condition from getting worse.
How long does it take to recover from cross linking?
How long does it take to recover from corneal cross-linking? Cross-Linking Recovery, the treated eye is usually painful for three to five days, levels of discomfort vary from patient to patient. Recovery time is about a week although most patients may find that it may be slightly longer.