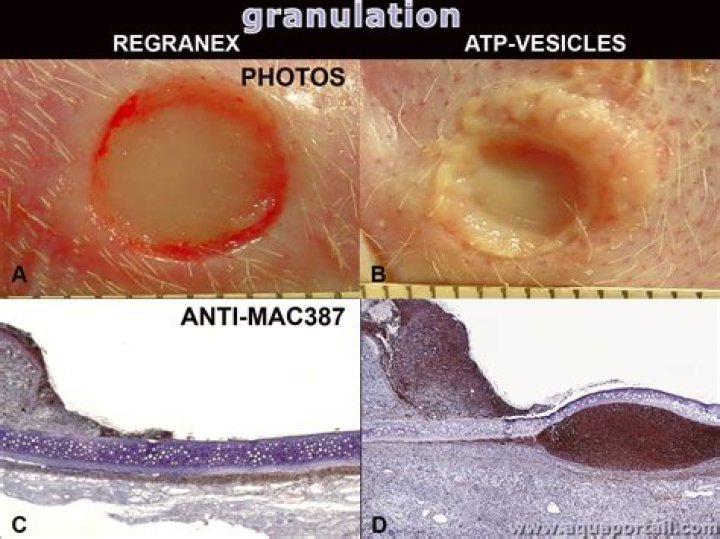
Is granulation tissue bad

Rachel Hickman
Published Feb 16, 2026
Healthy granulation tissue is pink in colour and is an indicator of healing. Unhealthy granulation is dark red in colour, often bleeds on contact, and may indicate the presence of wound infection. Such wounds should be cultured and treated in the light of microbiological results.
What is granulation tissue in a wound?
Granulation tissue is the primary type of tissue that will fill in a wound that is healing by secondary intention. It is made up of macrophages, which help to remove debris and release cytokines.
Does granulation tissue go away?
Granulation tissue will usually settle on its own and does not require any treatment. Granulation tissue can sometimes be treated in a perineal or gynaecology clinic with a painless procedure using silver nitrate.
How is granulation tissue treated?
Hypergranulation tissue can be treated with hypertonic salt water soaks, hydrocortisone cream, antimicrobial foam dressing or silver nitrate.Is granulation tissue painful?
Unlike healthy vaginal tissue, granulation tissue is often fibrotic and can cause local pain, inflammation, and bleeding. The presence of granulation tissue can also lead to pain and bleeding with intercourse, pelvic exam, or the use of tampons.
How long does it take for granulation tissue to go away?
This is granulation tissue and is necessary for healing. New pink skin will grow from the edge to the center of the wound, over this granulation tissue. The whole process may take 3-5 weeks depending on the size and depth of the wound. The area may remain numb for several weeks or even months.
Does granulation tissue bleed?
This gives granulation the appearance of red lumps (or granules) within the normal paler pink matrix, and despite this pink to red appearance, granulation does not bleed easily. Once the wound is filled with granulation tissue, it provides a foundation for re-epithelialization.
What stage of healing does granulation tissue?
The proliferative phase is characterized by the formation of granulation tissue, reepithelialization, and neovascularization. This phase can last several weeks.Should a healing wound be yellow?
If you have a scab, it’s considered normal to see it change into a yellowish color over time. This is completely normal and is the result of the hemoglobin from red blood cells in the scab being broken down and washed away.
What causes granulation?Granulation tissue formation is part of a normal healing process. Under certain conditions, such as infection, self-mutilation, or a local reaction to a chronically implanted, foreign material, this tissue grows uncontrollably and becomes very vascular and secretive.
Article first time published onWhat causes over granulation?
It is possible that overgranulation occurs due to the over-efficiency of modern day dressings or a possible infection that has prevented the ‘switching-on’ day following surgery (Collins et al, 2002). Due to the surgery and his poor general condition, the patient had lost more than two stone in weight.
Why granulation is required?
Why is Granulation Necessary? The granulation process allows particles to stick together more firmly. It increases the particle size of the constituents used, which are mostly very fine powders. The greater the particle size of a constituent, greater will be its compressive or binding ability.
What is granulation tissue made of?
The granulation tissue itself is made up of extracellular matrix, proteoglycans, hyaluronic acid, collagen, and elastin. Cytokines and growth factors, interleukins, and angiogenesis factors are active during this time, which can continue anywhere from days to weeks under normal circumstances.
How do you treat granulation tissue at home?
Another option for treatment is GranuLotion, an over-the-counter product that many parents use to help treat granulation tissue. Home remedies that may help include Tea Tree Oil, Maalox or another antacid, Calmoseptine Ointment, or aloe vera (fresh or gel form).
What dressing is used for Overgranulation?
In the management of overgranulation, topical antimicrobial products include povidone- iodine, cadexomer-iodine, silver and honey-based dressings (Leak, 2002; Hampton, 2007). Historically, caustic preparations have been used to ‘burn back’ overgranulation tissue.
When does granulation start?
Formation of Granulation Tissue At approximately 3 to 4 days following injury, a new stromal framework—known as granulation tissue—begins to enter the wound and replace the fibrin clot. Granulation tissue consists of a dermal matrix that provides a framework for cell migration, which is enhanced by angiogenesis.
How do you dress a granulating wound?
For deep cavity granulating wounds, a polyurethane foam dressing (eg, Allevyn, Lyofoam, Tielle) can be used to pack the wound. These usually consist of foam or foam chips enclosed within a soft flexible pouch to allow entry of exudates.
What color pus is bad?
Pus is a thick fluid that usually contains white blood cells, dead tissue and germs (bacteria). The pus may be yellow or green and may have a bad smell. The usual cause is an infection with bacteria.
How do you tell if your wound is infected?
- Warmth. Often, right at the beginning of the healing process, your wound feels warm. …
- Redness. Again, right after you’ve sustained your injury, the area may be swollen, sore, and red in color. …
- Discharge. …
- Pain. …
- Fever. …
- Scabs. …
- Swelling. …
- Tissue Growth.
How do I know if my wound is healing properly?
Even after your wound looks closed and repaired, it’s still healing. It might look pink and stretched or puckered. You may feel itching or tightness over the area. Your body continues to repair and strengthen the area.
Does itching mean healing?
Myth #9: Wounds itch when healing We all know the feeling: some time after an injury, the affected area will begin to tingle and itch. This goes especially for superficial wounds. And yes – in fact, this itching may indicate that the healing process is well on its way.
What are the 4 stages of healing?
The complicated mechanism of wound healing occurs in four phases: hemostasis, inflammation, proliferation, and remodeling.
Is it better to keep a wound covered or uncovered?
A: Airing out most wounds isn’t beneficial because wounds need moisture to heal. Leaving a wound uncovered may dry out new surface cells, which can increase pain or slow the healing process. Most wound treatments or coverings promote a moist — but not overly wet — wound surface.
What is granulation medicine?
Abstract. Granulation, the process of particle enlargement by agglomeration technique, is one of the most significant unit operations in the production of pharmaceutical dosage forms, mostly tablets and capsules. Granulation process transforms fine powders into free-flowing, dust-free granules that are easy to compress …
What does over granulation look like?
Hypergranulation (also known as over granulation or proud flesh) is a common non-life threatening phenomena. Hypergranulation is characterised by the appearance of light red or dark pink flesh that can be smooth, bumpy or granular and forms beyond the surface of the stoma opening.
What are the steps of granulation?
- Step 1: Weighing and mixing of formulation ingredients (excluding the lubricant). …
- Step 2: Preparing the damp mass. …
- Step 3: Wet screening/ Screening the dampened powder into pellets or granules. …
- Step 4: Drying of moist granules.
What is the principle of granulation?
Granulation is a process in which powder particles are made to adhere to each other, resulting in larger, multi-particle entities, so called granules. If such a process is performed without adding liquids, this is called dry granulation.
What do you mean by granulated?
: to form or crystallize into grains or granules. intransitive verb. : to form granulations an open granulating wound.
What replaces granulation tissue?
The extracellular matrix of granulation tissue is created and modified by fibroblasts. Initially, it consists of a network of type-III collagen, a weaker form of the structural protein that can be produced rapidly. This is later replaced by the stronger, long-stranded type-I collagen, as evidenced in scar tissue.