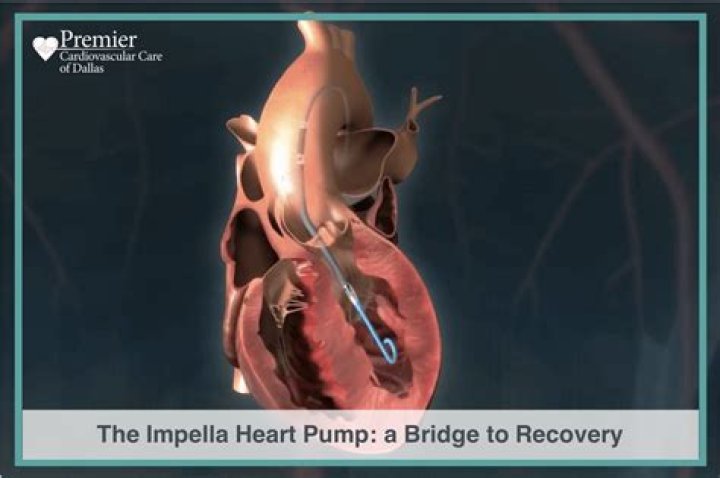
How does the Impella work

Sophia Edwards
Published Feb 12, 2026
The Impella pulls blood from the ventricle and pushes it out into the aorta, delivering oxygen-rich blood to the rest of your body. This allows your heart to rest while the doctor performs the PCI. Once the PCI procedure is complete, the Impella is turned off and guided out.
Why would a patient need an Impella?
Impella has been increasingly used in patients with: Severe heart failure – When the heart muscle is weak, blood cannot be pumped efficiently enough to get oxygen to all of the cells. Sometimes the heart becomes enlarged and weak. Other times it may be thick and stiff.
When do you use Impella?
Impella 2.5 is indicated for clinical use in cardiology and cardiac surgery for a number of indications. The primary indication is for cardiovascular support before, during and after urgent or elective high-risk percutaneous coronary intervention (PCI).
How long can you be on Impella?
The Impella RP System is indicated for providing temporary right ventricular support for up to 14 days in patients with a body surface area ≥1.5 m2, who develop acute right heart failure or decompensation following left ventricular assist device implantation, myocardial infarction, heart transplant, or open-heart …Can you do CPR on a patient with an Impella?
Cardiopulmonary support (CPR) should be initiated immediately per hospital protocol if indicated for any patient supported with the Impella® RP Catheter. When initiating CPR, reduce the Impella® RP Catheter flow rate.
Where does the Impella sit in the heart?
The Impella device is a catheter-based miniaturized ventricular assist device. Using a retrograde femoral artery access, it is placed in the left ventricle across the aortic valve.
Does Impella need anticoagulation?
The Impella heart pumps require a specific purge pressure range (300-1100 mm Hg) for optimal pump flow and a specific systemic ACT anticoagulation range (160-180 seconds) for optimal and sustained function.
How do you implant impella?
The standard technique for the implantation of Impella CP involves insertion of the percutaneous femoral artery introducer for the guidewire to be advanced via the aorta and aortic valve into the left ventricle under fluoroscopy. The microaxial pump is then implanted using modified Seldinger technique.What is the Impella heart pump?
The Impella heart pump is the world’s smallest heart pump used to help maintain blood flow during high-risk protected percutaneous coronary interventions (PCI).
What is the success rate of LVAD surgery?Patient Survival The overall survival on LVAD support was 86.1%, 56.0%, and 30.9% at 30 days, 1 year, and 2 years after LVAD implantation, respectively, as shown in Figure 1. A total of 155 of 280 patients (55%) died during the mean support time of 10.4 months (range, 1 day to 3.6 years).
Article first time published onWhat is the name of the heart pump?
Left ventricular assist device (LVAD) A ventricular assist device (VAD) — also known as a mechanical circulatory support device — is a device that helps pump blood from the lower chambers of your heart (ventricles) to the rest of your body.
How do you wean impella?
To initiate weaning, reduce P level in 2 level increments (eg, P-8 to P-6 to P-4) as hemodynamics tolerate. Keep Impella at P-2 until you are ready to explant the device from the left ventricle. Once hemodynamics allow—CVP~10-12, CI>2—pull the catheter from the left ventricle into the aorta at P-2.
Why do LVAD patients have no pulse?
An impeller within the pump spins thousands of times a minute, resulting in continuous blood flow, which means LVAD patients don’t have a pulse or measurable blood pressure. The external components include a controller—the brains of the system—and batteries, which power the system.
What does Rp stand for in Impella RP?
Explore Impella RP® Heart Pump for Right-Sided Heart Recovery. Impella RP®
What is the difference between IABP and Impella?
The Impella heart pump is placed in the left ventricle, the main pumping chamber of your heart. It delivers blood from your heart into the aorta, the main blood vessel carrying blood to your body. This provides blood your body needs while allowing the heart to rest. The IABP is placed in your aorta.
When removing the peel away sheath to place the repositioning sheath It is important to peel the sheath completely prior to removing from the body?
Flush the sidearm of the peel-away introducer and ensure the sheath is completely out of the body prior to peeling it away. If using the 14Fr x 25cm peel-away sheath for the Impella CP, it may be necessary to push the sheath over the repositioning sheath to fully remove from the body prior to peeling it away.
Who invented the Impella?
Thorsten Siess, PhD, Abiomed’s chief technology officer and inventor of Impella® discusses how the world’s smallest heart pump transformed from a product to a platform.
How is impella flow calculated?
LVEDP is calculated using the pressure assessed in the aorta from the optical sensor and the pressure derived from the motor. The Impella CP with SmartAssist is designed to run at a constant motor speed in response to the real-time changes in pressures in the aorta and left ventricle.
Is an Impella device a VAD?
Impella (Abiomed, Danvers, MA) is a percutaneously inserted ventricular assist device (VAD). It has been increasingly used in patients with severe heart failure, cardiogenic shock, and high-risk percutaneous intervention (PCI).
How is the Impella 5.0 catheter inserted?
Impella 5.0 is inserted through the axillary artery or femoral cut down. Benefits include: Immediately ambulate patients. Resting the left ventricle has proven to increase heart recovery while keeping other therapeutic options open.
What is a tandem heart?
The TandemHeart is a left atrial-to-femoral artery bypass system comprising a transseptal cannula, arterial cannulae, and a centrifugal blood pump. The pump can deliver flow rates up to 4.0 L/min at a maximum speed of 7500 rpm.
What is the leading cause of death for LVAD patients?
Methods and Results— Of 89 patients who died with a DT-LVAD, the median (25th–75th percentile) time from left ventricular assist device implantation to death was 14 (4–31) months. The most common causes of death were multiorgan failure (26%), hemorrhagic stroke (24%), and progressive heart failure (21%).
What is the longest someone has lived with an LVAD?
David Pierce has the distinguished recognition of being the longest living HeartMate II LVAD patient in the U.S. David received his first LVAD on May 26, 2004, at the age of 52. Today, he is living a happy, healthy life — and spending precious time with his family.
How long is hospital stay after LVAD surgery?
On average patients remain in the hospital for 14 – 21 days after LVAD implantation. During this time you and your caregivers will begin learning about your new device.
What does CRT stand for in cardiology?
Cardiac resynchronization therapy (CRT) is treatment to help your heart beat with the right rhythm. It uses a pacemaker to restore the normal timing pattern of the heartbeat. The CRT pacemaker coordinates how timing of the upper heart chambers (atria) and the lower heart chambers (ventricles).
What sends blood back to the heart?
Oxygen-poor blood returns from the body to the heart through the superior vena cava (SVC) and inferior vena cava (IVC), the two main veins that bring blood back to the heart. The oxygen-poor blood enters the right atrium (RA), or the right upper chamber of the heart.
Is LVAD a pacemaker?
Compared with a pacemaker An LVAD and a pacemaker serve different purposes. While an LVAD helps the heart pump blood effectively, a pacemaker helps correct an irregular or slow heartbeat. It does not help with pumping — instead, a pacemaker generates electrical stimulation that regulates the heartbeat.
What are the Act recommendations for the Impella RP device?
Gradually increase the performance levels to achieve optimal flow and hemodynamic support. Impella Patient Management: Maintain ACT at 160-180 sec for a duration of Impella RP support (> 250 sec at time of insertion).
Can you take BP with LVAD?
Patients with LVADs often do not have a palpable pulse, and therefore traditional BP measurement by auscultation or automated cuff is less reliable.
Can you take BP on LVAD patient?
Since LVAD patients do not typically have palpable peripheral pulses and blood pressures that can be measured by automated cuffs, first use US to get your patient’s MAP. Attach a manual BP cuff to your patient’s arm, inflate > 120 mm Hg, then slowly deflate it while having the Doppler US probe over the brachial artery.
Can you check BP with LVAD?
In addition, due to their improved durability, continuous flow LVADs otherwise known as CF-VAD are predominately replacing pulsatile LVADs. An essential component of optimal clinical care is the accurate measurement of blood pressure (BP) as well as the recognition and management of hypertension in patients with LVADs.



