How do you use lavage NGT

Mia Kelly
Published Feb 12, 2026
Insert the nasogastric/orogastric tube into the stomach, then confirm placement (see Nasogastric/Orogastric Tube Insertion). … Introduce 200 to 300 mL of water at body temperature into the tube and then lower the tube into the bucket below the level of the stomach before water disappears from the funnel.
What is a lavage procedure?
Gastric lavage involves placing a tube through the mouth (orogastric) or through the nose (nasogastric) into the stomach. Toxicants are removed by flushing saline solutions into the stomach, followed by suction of gastric contents.
What is gastric lavage nursing?
Gastric lavage is the washing out of the stomach via a nasogastric tube or stomach tube. Lavage is ordered to wash out the stomach (after ingestion of poison or an overdose of medication, for example) or to control gastrointestinal bleeding.
When is gastric lavage used?
Apart from toxicology, gastric lavage (or nasogastric lavage) is sometimes used to confirm levels of bleeding from the upper gastrointestinal tract. It may play a role in the evaluation of hematemesis. It can also be used as a cooling technique for hyperthermic patients.What is the purpose of the ice water lavage?
Gastric hypothermia by lavage of the stomach with iced water or saline is believed by many to be the safest and simplest way to reduce bleeding from the stomach.
What does lavage mean in medical terms?
(luh-VAZH) In medicine, washing out an organ (such as the stomach or colon), a body cavity, or a wound by flushing it with a fluid.
Why is lavage used for therapy of hypo and hyperthermia?
Because gastric mucosa does not significantly vasoconstrict and the stomach lies in close proximity to the liver and inferior vena cava, gastric lavage is a reasonable method to rapidly cool hyperthermic patients. A core temperature reduction of approximately 0.15°C per minute can be achieved using this method.
What are the complications of gastric lavage?
Complications of gastric lavage include aspiration pneumonia, charcoal aspiration, laryngospasm, inadvertent tracheal intubation, and respiratory insufficiency [11,12]. Placement of the tube can increase vagal tone and may cause a life-threatening bradydysrhythmia.Does gastric lavage prevent vomiting?
Gastric lavage in neonates with MSAF is still a routine practice in neonatal units in order to avoid vomiting and subsequent aspiration of meconium and gastric contents.
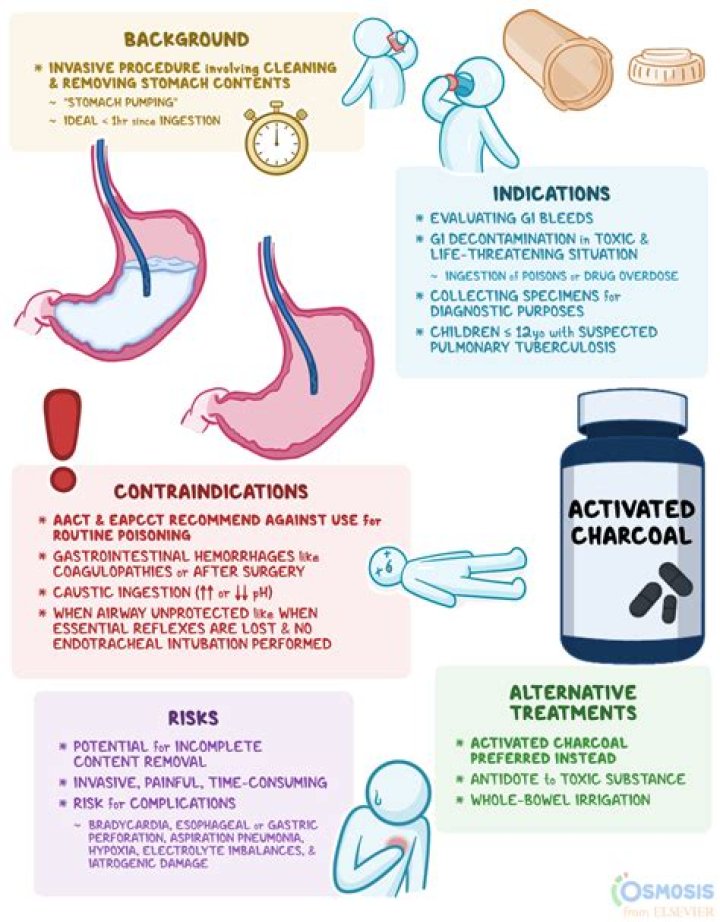
What are the contraindications of gastric lavage?Contraindications include loss of protective airway reflexes (unless the patient is first intubated tracheally), ingestion of a strong acid or alkali, ingestion of a hydrocarbon with a high aspiration potential, or risk of GI hemorrhage due to an underlying medical or surgical condition.
Article first time published onWhat equipment is needed for gastric lavage?
Nasogastric tube. Ice water. Endotracheal intubation equipment, if airway needs to be protected (see Rapid Sequence Intubation) Y connector.
What are the necessary assessment done before performing the gastric lavage?
Before the procedure, assess and document the patient’s level of consciousness (LOC) and obtain and record vital signs. Assess for and document any contraindications to gastric lavage, such as decreased LOC with an unprotected airway. Document patient teaching provided.
What is gastric lavage with ice water?
GASTRIC LAVAGE with iced water has long been used in the management of upper gastrointestinal hemorrhage. The vasoconstrictive effect of cooling and the clinical impression of its efficacy have led to refinements in the technique of cooling and more exact evaluation of its physiological effects.
What is ice gastric lavage?
Cold saline gastric lavage in acute upper gastroin- testinal hemorrhage serves several purposes. It gives information on the rate of bleeding and con- trol. It promotes hemostasis by decreasing gastro- duodenal blood flow and portal pressure [I].
Where do you put cold packs for hyperthermia?
Place ice packs in the patient’s groin and in the axillae. Ice packs around the neck should be avoided to prevent interference with thermoregulation in the brain. Remove ice packs once core temperature reaches 39°C.
What should you never do when treating hyperthermia?
Use cold wet towels or dampen clothing with tepid water when the heat is extreme. Avoid hot, heavy meals. Avoid alcohol. Determine if the person is taking any medications that increase hyperthermia risk; if so, consult with the patient’s physician.
What is the most effective method for treating hyperthermia?
The definitive treatment for heat-related illness is total body cooling. Conduction and evaporation are the two modes of cooling employed in the treatment of heat-related illness. Studies have shown ice-water immersion to be the most rapidly effective.
What is a lavage kit?
A kit designed for use in common gastric emergency conditions where quick and effective lavage or flushing of the stomach is required, (e.g. gastric dilatation volvulus and acute poisonings). The kit includes 3 large bore semi-rigid lavage tubes and a stomach irrigation system that connects to any faucet.
How is diagnostic peritoneal lavage done?
Diagnostic peritoneal lavage (DPL) is an invasive emergency procedure used to detect hemoperitoneum and help determine the need for laparotomy following abdominal trauma. A catheter is inserted into the peritoneal cavity, followed by aspiration of intraperitoneal contents, often after their dilution with crystalloid.
Is ipecac still used?
In the past, ipecac syrup was commonly used to cause vomiting in people who ingested poison. But now it is no longer recommended. It doesn’t seem to work better than activated charcoal, another agent used for poisoning.
What can cause meconium aspiration?
Meconium aspiration syndrome occurs when stress (such as infection or low oxygen levels) causes the fetus to take forceful gasps, so that the amniotic fluid containing meconium is breathed (aspirated) in and deposited into the lungs.
How do you wash a baby's stomach?
Dip a cotton swab in warm water. Squeeze the tip to remove the excess water. Gently clean around the base of the cord and then the surrounding skin, then hold the stump with a clean absorbent cloth to dry it completely. It is important that the umbilical cord remain clean and dry until it falls off naturally.
Which adverse drug reaction is managed by gastric lavage?
Gastric lavage has been used to manage toxic ingestions since the early 1800s.
What is gastric dumping?
Dumping syndrome is a medical condition in which your stomach empties its contents into the first part of your small intestine (the duodenum) faster than normal. Dumping syndrome is also known as rapid gastric emptying. People with dumping syndrome experience symptoms like nausea and abdominal cramping.
What is gastric aspirate?
Gastric aspiration is a technique used to collect gastric contents that can be used in the diagnosis of tuberculosis. Tuberculosis continues to be a problem and children are dispro- portionately affected, in part because they are more likely to get sick when they are infected with the TB organism.
How do you check NG tube placement ATI?
Assess tube placement by looking the mark below the naris. Using syringe, withdraw gastric contents, assess aspirate, and test pH. Draw irrigation solution into syringe and slowly instill into tube. Reconnect nasogastric tube to suction.
Why charcoal is used in gastric lavage?
Activated charcoal is now being recommended for patients who have ingested potentially toxic amounts of a poison, where the ingested substance adsorbs to charcoal.
Can a nurse perform gastric lavage?
Gastric lavage is typically done in the emergency department or on the intensive care unit by a doctor, gastroenterologist, or nurse; a wide-bore lavage tube is almost always inserted by a gastroenterologist.