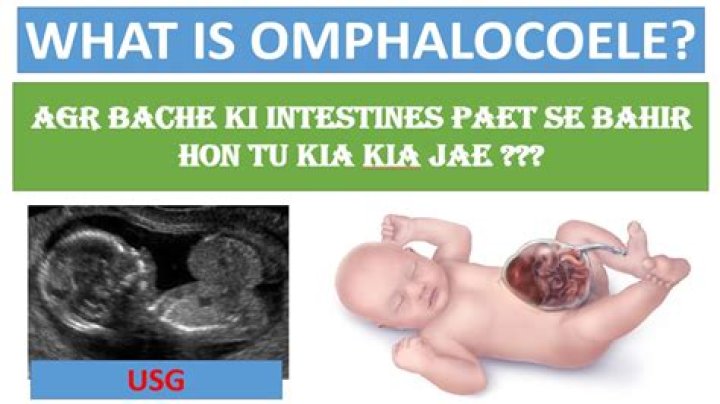
How do you fix omphalocele

Mia Morrison
Published Apr 11, 2026
The repair is performed the following way: Right after birth, a plastic pouch (called a silo) or a mesh-type of material is used to contain the omphalocele. The pouch or mesh is then attached to the baby’s belly. Every 2 to 3 days, the doctor gently tightens the pouch or mesh to push the intestine into the belly.
Can omphalocele correct itself?
Small omphaloceles are often fixed easily. They normally cause no long-term problems. Babies with damage to the abdominal organs may have long-term problems.
What causes an omphalocele?
Omphalocele is a feature of many genetic syndromes. Nearly half of individuals with omphalocele have a condition caused by an extra copy of one of the chromosomes in each of their cells (trisomy). Up to one-third of people born with omphalocele have a genetic condition called Beckwith-Wiedemann syndrome.
Is omphalocele an emergency?
Omphalocele repair surgery will be needed to repair the hole in the abdominal wall. Omphalocele surgery is not an emergency and is usually done within a couple days after birth.What major is omphalocele?
Español (Spanish) Omphalocele (pronounced uhm-fa-lo-seal) is a birth defect of the abdominal (belly) wall. The infant’s intestines, liver, or other organs stick outside of the belly through the belly button. The organs are covered in a thin, nearly transparent sac that hardly ever is open or broken.
Can you live with omphalocele?
Living with an omphalocele After surgery, your baby may still be at risk for long-term issues. Your baby’s chance for future problems depends on: The size of the omphalocele. If part of the intestine or other organs lost blood flow.
How serious is omphalocele?
The survival rate for babies who have an omphalocele and serious problems with other organs is about 70 percent. Your baby may also have some feeding difficulty, reflux, growth delays and bowel obstruction and could have long-term breathing problems. Your baby may be more prone to sickness than other babies.
Is omphalocele worse than gastroschisis?
Care should be taken to investigate fully for associated congenital anomalies, especially in a child with a large omphalocele, which frequently is accompanied by congenital cardiac defects. Children with gastroschisis will tend to have greater problems with bowel function than patients with omphaloceles.Is omphalocele a hernia?
Exomphalos (omphalocele) Exomphalos is characterized by herniation of the intra-abdominal contents into the base of the umbilical cord, with a covering amnioperitoneal membrane. The most frequently herniated organs are the liver, bowel and stomach.
What is a ruptured omphalocele?Omphalocele is an abdominal wall defect which can be classified as small, giant, or ruptured. Ruptured omphaloceles require prompt diagnosis and management to prevent associated morbidity and mortality and represent a challenging surgical condition.
Article first time published onWhat is it called when your born with your intestines on the outside?
Español (Spanish) Gastroschisis (pronounced gas-troh-skee-sis) is a birth defect of the abdominal wall. The baby’s intestines are found outside of the baby’s body, exiting through a hole beside the belly button.
What does Exomphalos mean?
Exomphalos is an abdominal wall (tummy wall) defect. It happens when a baby’s abdominal wall does not develop fully while in the womb. Early in all pregnancies, the baby’s intestine develops inside the umbilical cord. It usually moves inside the abdomen a few weeks later.
Is omphalocele more common in males?
A small type of omphalocele that involves only the protrusion of the intestines occurs in one in 5,000 babies, whereas a large type that sees a protrusion of the intestines, liver, and other abdomen organs happens to one in 10,000 babies. Boys have an omphalocele more often than girls.
What medication causes omphalocele?
Women who use tobacco while pregnant are at an increased risk of their unborn child developing omphalocele. SSRIs. Women who use selective serotonin-reuptake inhibitors (SSRIs) during pregnancy are more likely to have a baby with omphalocele. SSRIs are usually found in medications like antidepressants.
Can omphalocele be misdiagnosed?
One omphalocele case was undiagnosed prenatally due to lack of prenatal care. Five cases of omphalocele were misdiagnosed on fetal sonogram as gastroschisis. Conversely, there were two cases of gastroschisis misdiagnosed as omphalocele on fetal sonogram.
Is omphalocele associated with Malrotation?
Omphalocele is caused by malrotation of the bowels while returning to the abdomen during development. Some cases of omphalocele are believed to be due to an underlying genetic disorder, such as Edward’s syndrome (trisomy 18) or Patau syndrome (trisomy 13).
Can omphalocele be diagnosed at 11 weeks?
With the introduction of first trimester ultrasound (US) screening of nuchal translucency for Down syndrome, the prenatal diagnosis of congenital anomalies is now feasible as early as 11–14 weeks of gestation [3]. An early gestational scan at 11–14 weeks may be able to detect fetal omphalocele simultaneously [3].
How early can omphalocele be detected?
The earliest that an omphalocele can be detected is at 12 weeks of menstrual age.
What is the difference between gastroschisis and omphalocele?
In gastroschisis, the opening is near the bellybutton (usually to the right) but not directly over it, like in omphalocele. Like in omphalocele, the opening allows the intestines to spill out but unlike omphalocele, the intestines are not covered by a thin sac.
What are the long term effects of omphalocele?
Small omphaloceles normally cause no long-term problems. Babies with damage to the abdominal organs may have long-term problems. Your child may have trouble with digestion, having bowel movements, and infection.
What is the difference between umbilical and Paraumbilical hernia?
A direct or true umbilical hernia consists of a symmetric protrusion through the umbilical ring and is seen in neonates or infants. Indirect umbilical (paraumbilical) hernias protrude above or below the umbilicus and are the most common type of umbilical hernia in adults.
What is associated with omphalocele?
Omphalocele can be associated with single gene disorders, neural tube defects, diaphragmatic defects, fetal valproate syndrome, and syndromes of unknown etiology.
Which has better prognosis omphalocele or gastroschisis?
Because the peritoneal sac is absent, the fetal bowel is continuously exposed to the amniotic fluid, resulting in significant inflammation of the bowel wall [2]. Omphalocele is known to have more associated anomalies and higher mortality rate than gastroschisis [2].
Can a baby be born without a belly button?
“It’s sort of crinkly and creates the appearance of a belly button.” Babies who have an omphalocele, on the other hand, truly are born without a belly button. The intestines or other abdominal organs protrude through a hole in the middle of the baby’s abdomen, right where the belly button would be.
Why some people don't have a belly button?
Some people don’t have a belly button, and the reason for this may be related to surgical history or just an anomaly in how the belly button formed (or didn’t, for that matter). Most of the time, if you don’t have a belly button, it’s related to a surgery or a medical condition you had when you were younger.
Can a baby survive without an umbilical cord?
In these early weeks, there’s no need to breathe. The umbilical cord is the main source of oxygen for the fetus. As long as the umbilical cord remains intact, there should be no risk of drowning in or outside the womb.
How is exomphalos diagnosed?
Exomphalos is usually detected at the 18+0−20+6 weeks Fetal Anomaly ultrasound scan. It can be diagnosed by ultrasound earlier in pregnancy however the condition is not usually diagnosed before 11 weeks. This is due to the physiological herniation of the bowel into the umbilical cord during early fetal development.
What is the difference between gastroschisis and exomphalos?
Infants with exomphalos usually have an associated non-rotation or malrotation of their intestine. The liver, spleen, and ovaries are frequently present in the sac. Gastroschisis is a smaller defect in the abdominal wall, located to the right side of the anatomically normal umbilical cord.
How often is omphalocele isolated?
The presence of isolated omphalocele without association to genetic defect or associated structural anomaly is estimated in 3–6.5% of all cases when it is prenatally diagnosed [3, 7].
What is ventral wall defects?
Ventral abdominal body wall defects comprise a group of congenital malformations that includes gastroschisis and omphalocele, which are relatively common, and ectopia cordis, bladder exstrophy, and cloacal exstrophy, which are extremely rare.