How do you calculate ARDS

Robert Spencer
Published Feb 21, 2026
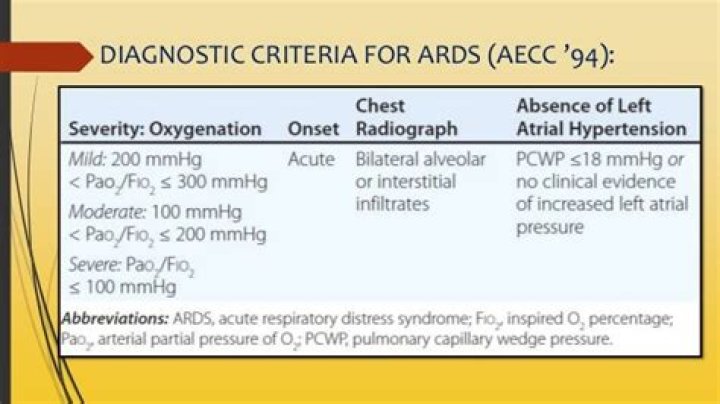
The severity of the ARDS is defined by the degree of hypoxemia, which is calculated as the ratio of arterial oxygen tension to fraction of inspired oxygen (PaO2/FiO2).
How do you calculate the sao2 FiO2 ratio?
How to Calculate FIO2 from Liters. Example: A patient has a pO2 of 85mmHg on ABG while receiving 5 liter/minute of oxygen. 5 L/min = 40% oxygen = FIO2 of 0.40, the P/F ratio = 85 divided by 0.40 = 212.5.
How do you calculate pa02 fi02 ratio?
PaO2 should = FiO2 x 500 (e.g. 0.21 x 500 = 105 mmHg)
What is PF ratio in ARDS?
The current Definition of ARDS for Oxygenation is P/F Ratio of 300 to 200 is Mild, 200 to 100 is Moderate and less than 100 is Severe ARDS with PEEP ≥ 5.How is PF ratio calculated without ABG?
If your patient’s spo2 = 90%, your patient’s PaO2=60mmHg. If your patient’s spo2=99%, your patient’s PaO2=90mmHg. So if your patient’s SpO2 = 97% and the FiO2=40%, you can estimate the P/F ratio as ~80/0.4=200.
What is the difference between PaO2 and SpO2?
PaO2 values are always much lower than oxygen saturation values. This is simply a reflection of the oxygen saturation curve (figure above). For example, a saturation of 88% correlates to a PaO2 of ~55mm. We’re generally comfortable with a saturation of 88%, but a PaO2 of 55mm may cause concern.
What is ARDS scale?
According to the Berlin definition, the acute respiratory distress syndrome (ARDS) is classified as mild, moderate, and severe by using an arterial partial pressure of oxygen (PaO2) to fraction of inspired oxygen (FIO2) threshold of 300, 200, and 100 mm Hg, respectively (1).
What would the PaO2 be for a patient with an SpO2 of 90?
On the OHDC, a SaO2 value of 90% correlates to a PaO2 level of 60 mm Hg.What is SpO2 and FiO2?
Association Between Peripheral Blood Oxygen Saturation (SpO2)/Fraction of Inspired Oxygen (FiO2) Ratio Time at Risk and Hospital Mortality in Mechanically Ventilated Patients. Save.
How is pO2 calculated?It is not possible to collect gases directly from the alveoli. The alveolar gas equation is of great help in calculating and closely estimating the partial pressure of oxygen inside the alveoli. The alveolar gas equation is used to calculate alveolar oxygen partial pressure: PAO2 = (Patm – PH2O) FiO2 – PACO2 / RQ.
Article first time published onWhat is Peep measured in?
This pressure is typically achieved by maintaining a positive pressure flow at the end of exhalation. This pressure is measured in centimeters of water.
Is PO2 the same as PaO2?
PO2 is just partial pressure of oxgen in a given environment, such as room air. … PAO2 is partial pressure of oxygen in alveoli. PaO2 is partial pressure of oxygen dissolved in (arterial) blood. Partial pressure of a gas dissolved in a liquid depends on the qualities of the liquid and the concentration of the gas.
What does FIO2 0.5 mean?
Fraction of inspired oxygen (FIO2), corrected denoted with a capital “I”, is the molar or volumetric fraction of oxygen in the inhaled gas. … FIO2 is typically maintained below 0.5 even with mechanical ventilation, to avoid oxygen toxicity, but there are applications when up to 100% is routinely used.
What is FIO2 of 2l nasal cannula?
At 2 LPM, the approximate FiO2 is 28%.
How is PF calculated?
The employee contributes 12 percent of his or her basic salary along with the Dearness Allowance every month to the EPF account. For example: If the basic salary is Rs. 15,000 per month, the employee contribution shall be 12 % of 15000, which comes to Rs 1800/-. This amount is the employee contribution.
What is fi02 on a ventilator?
FiO2: Percentage of oxygen in the air mixture that is delivered to the patient. Flow: Speed in liters per minute at which the ventilator delivers breaths. Compliance: Change in volume divided by change in pressure.
What are the 3 phases of ARDS?
In ARDS, the injured lung is believed to go through three phases: exudative, proliferative, and fibrotic, but the course of each phase and the overall disease progression is variable.
What is the difference between ABG and pulse oximeter?
Arterial blood gas tests are invasive, requiring a blood sample, and provide information at a specific moment in time. Pulse oximetry is not invasive. It uses a sensor attached to the person’s finger. It can also provide continuous measurements of the amount of oxygen in the blood.
Is SaO2 or SpO2 more accurate?
ABGArterial Blood GasesSao2Saturation of Oxygen (arterial blood)Spo2Spot Oxygen Saturation
What SpO2 is considered hypoxic?
Lower than 92% is considered hypoxic. For patients with COPD, oxygen saturation levels may range from 88% to 92%. Lower than 88% is considered hypoxic. Patients who are hypoxic may breathe differently, which may signal the need for supplemental oxygen.
What is a good oxygen saturation?
A normal level of oxygen is usually 95% or higher. Some people with chronic lung disease or sleep apnea can have normal levels around 90%. The “SpO2” reading on a pulse oximeter shows the percentage of oxygen in someone’s blood. If your home SpO2 reading is lower than 95%, call your health care provider.
What is the relationship between SpO2 and PaO2?
SpO2 correlated well with arterial pO2 as predicted by the standard oxygen-hemoglobin dissociation curve in a undifferentiated critically ill patient population. In this study, a SpO2 >90% correlated with an arterial pO2 >60 mmHg more than 94% of the time.
Which is more important SaO2 or PaO2?
PaO2 is the most important (but not the only) determinant of SaO2. Other determinants of SaO2 for a given PaO2 are conditions that shift the position of the oxygen dissociation curve left or right, such as temperature, pH, PaCO2 and level of 2,3-DPG in the blood.
How do you read PaO2?
- Normal PaO2 values = 80-100 mmHg.
- Estimated normal PaO2 = 100 mmHg – (0.3) age in years.
- Hypoxemia is PaO2 < 50 mmHg.
What would PO2 be on 100 oxygen?
For example, at sea level with no additional supplemental oxygen and a normal physiological state, the PO2 inside the alveoli calculates at approximately 100 mm Hg. But, if a patient is given 100% oxygen in the same situation the PO2 can be as high as 663 mm Hg.
What is normal range for PO2?
The PaO2 measurement shows the oxygen pressure in the blood. Most healthy adults have a PaO2 within the normal range of 80–100 mmHg. If a PaO2 level is lower than 80 mmHg, it means that a person is not getting enough oxygen .
How is PEEP calculated?
- Ensure the Paw waveform is displayed.
- Open the Hold window.
- Wait until the Paw waveform plot restarts from the left side.
- Wait for the next inspiration.
- Then select EXP hold.
- When the flow reaches zero, deactivate the hold maneuver by selecting EXP hold again.
What does a PEEP of 5 mean?
A higher level of applied PEEP (>5 cmH2O) is sometimes used to improve hypoxemia or reduce ventilator-associated lung injury in patients with acute lung injury, acute respiratory distress syndrome, or other types of hypoxemic respiratory failure.
What is normal PEEP value?
Applying physiologic PEEP of 3-5 cm water is common to prevent decreases in functional residual capacity in those with normal lungs. The reasoning for increasing levels of PEEP in critically ill patients is to provide acceptable oxygenation and to reduce the FiO2 to nontoxic levels (FiO2< 0.5).
What is difference between SaO2 and SpO2?
The mean difference between SpO2 and SaO2 was -0.02% and standard deviation of the differences was 2.1%. From one sample to another, the fluctuations in SpO2 to arterial saturation difference indicated that SaO2 could not be reliably predicted from SpO2 after a single ABG.
What is PCO2 in ABG?
The partial pressure of carbon dioxide (PCO2) is the measure of carbon dioxide within arterial or venous blood. It often serves as a marker of sufficient alveolar ventilation within the lungs. Generally, under normal physiologic conditions, the value of PCO2 ranges between 35 to 45 mmHg, or 4.7 to 6.0 kPa.