Does TPN increased glucose

Mia Kelly
Published Mar 28, 2026
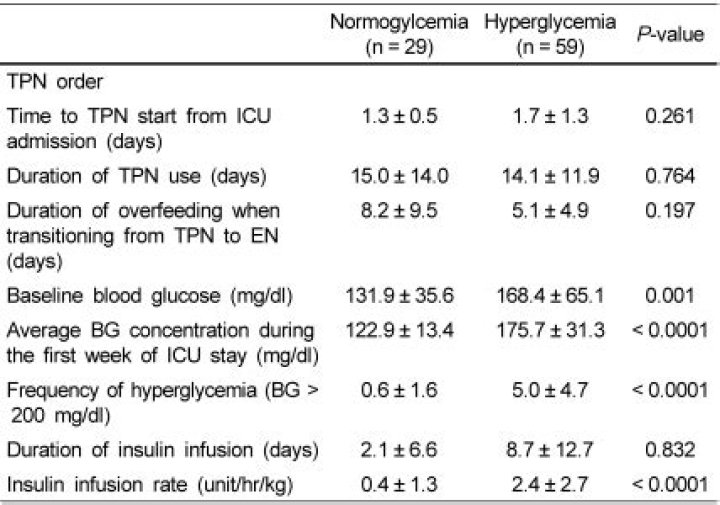
The mean blood glucose level before TPN was 123.2 ± 33 mg/dl and increased to a mean blood glucose of 146 ± 44 mg/dl within 24 h of TPN and remained elevated (147 ± 40 mg/dl) during days 2–10 of TPN infusion (P < 0.01 from baseline).
Does TPN cause high glucose?
The increased risk of complications during TPN therapy can be related, among other factors, to the development of hyperglycemia, which occurs in 10–88% of hospitalized patients receiving TPN therapy (4–6).
Does TPN cause hypoglycemia or hyperglycemia?
Objective: Treatment of hyperglycemia with insulin is associated with increased risk of hypoglycemia in type 2 diabetes mellitus (T2DM) patients receiving total parenteral nutrition (TPN).
Does TPN affect glucose?
In conclusion, our study showed that the amount of dextrose delivered via TPN might be associated with the development of hyperglycemia and poor clinical outcomes in critically ill patients without a history of diabetes mellitus and should be adapted carefully to maintain blood glucose within the target range.Does TPN cause hypoglycemia?
The total number of hypoglycemic episodes per 100 d of TPN was 0.82. In univariate analysis, hypoglycemia was significantly associated with the presence of diabetes, a lower body mass index (BMI), and treatment with intravenous (IV) insulin.
How often do you check blood glucose with TPN?
Conclusion. After 36 hours of TPN, we recommend decreasing testing to twice a day (AM serum glucose and CBG 12 hours later) in patients without preexisting diabetes and those stable medically.
How does TPN manage hyperglycemia?
Insulin Therapy During Total Parenteral Nutrition Insulin is the treatment of choice to control hyperglycemia during TPN. Both subcutaneous and intravenous insulin have been shown to be effective in managing hyperglycemia in these patients [13, 77].
Why is blood glucose monitoring necessary for a patient who is receiving TPN?
Conclusions: In non-diabetic cases, there is a risk of hyperglycemia during TPN even under appropriate nutritional management. It’s necessary for risk management to mesure periodic blood glucose.What is TPN diabetes?
Research published by the American Diabetes Association shows that non-critically ill patients who develop hyperglycemia or a high blood sugar after receiving total parental nutrition (TPN) or hyperalimentation are more likely to die in the hospital.
What are the side effects of TPN?- Dehydration and electrolyte Imbalances.
- Thrombosis (blood clots)
- Hyperglycemia (high blood sugars)
- Hypoglycemia (low blood sugars)
- Infection.
- Liver Failure.
- Micronutrient deficiencies (vitamin and minerals)
How can TPN prevent hypoglycemia?
- Monitor your blood sugar. …
- Don’t skip or delay meals or snacks. …
- Measure medication carefully, and take it on time. …
- Adjust your medication or eat additional snacks if you increase your physical activity. …
- Eat a meal or snack with alcohol, if you choose to drink. …
- Record your low glucose reactions.
What should I monitor for TPN?
Weight, complete blood count, electrolytes, and blood urea nitrogen should be monitored often (eg, daily for inpatients). Plasma glucose should be monitored every 6 hours until patients and glucose levels become stable. Fluid intake and output should be monitored continuously.
How does hyperglycemia occur?
What is hyperglycemia? Hyperglycemia, or high blood glucose, occurs when there is too much sugar in the blood. This happens when your body has too little insulin (the hormone that transports glucose into the blood), or if your body can’t use insulin properly. The condition is most often linked with diabetes.
Should TPN be continued during surgery?
TPN is usually slowed or discontinued prior to anesthesia, primarily to avoid complications from excessive (hyperosmolarity) or rapid decrease (hypoglycemia) in infusion rates in the busy operative arena. That said, because abrupt discontinuance may lead to severe hypoglycemia, TPN must be turned down gradually.
When can you stop parenteral nutrition?
Guidelines suggest that when tolerance to enteral nutrition is evident, parenteral nutrition should be weaned and discontinued when >60 percent of the patients’ needs are met enterally, although there are no data to support this practice [1].
Can tube feeding cause hypoglycemia?
Reactive hypoglycemia occurs following a postprandial insulin peak when there is insufficient substrate influx to sustain blood glucose levels. Post gastrectomy patients who are receiving enteral nutrition via direct jejunal feeding may be particularly at risk because they are often bedridden and do not complain.
What type of insulin is added to TPN?
Insulin is not routinely added to all TPN solutions. For patients who require insulin prior to the initiation of TPN, one-third to one-half of the usual total daily dose can be added to the TPN bag as regular human insulin. Depending on blood glucose levels, additional subcutaneous insulin may be administered.
How much insulin is in TPN?
Average total daily insulin dose was 17 ± 20 units before starting TPN and 53 ± 54 units on the last day of TPN. Patients received an average of 0.7 Units/kg total daily dose of insulin on the last day of TPN.
Why is total parenteral nutrition used?
Parenteral nutrition, often called total parenteral nutrition, is the medical term for infusing a specialized form of food through a vein (intravenously). The goal of the treatment is to correct or prevent malnutrition.
What is the most common complication of TPN?
The most common complications associated with TPN is central line infection. Other common complications include abnormal glucose levels and liver dysfunction. TPN use can lead to hyperglycemia, and stopping suddenly can cause hypoglycemia.
Why does TPN cause liver failure?
Nutrient Deficiencies. Patients who begin TPN because of severe protein malnutrition (Kwashiokor) may develop hepatic steatosis because of decreased very low density lipoprotein synthesis.
Can TPN cause elevated BUN?
2. Abnormalities of serum electrolytes and minerals Elevated BUN may reflect dehydration, which can be corrected by giving free water as 5% dextrose via a peripheral vein.
Which type of insulin acts most quickly?
TypeExamplesThe time of greatest effect (peak)Rapid-actingApidra (insulin glulisine)1–1.5 hoursFiasp (faster-acting insulin aspart)0.5–1.5 hoursHumalog (insulin lispro)1–2 hours
What is normal glucose level?
A blood sugar level less than 140 mg/dL (7.8 mmol/L) is normal. A reading of more than 200 mg/dL (11.1 mmol/L) after two hours indicates diabetes. A reading between 140 and 199 mg/dL (7.8 mmol/L and 11.0 mmol/L) indicates prediabetes.
What's the difference between TPN and PPN?
Total Parenteral Nutrition (TPN) is the delivery of nutrients sufficient to meet metabolic requirements. Peripheral Parenteral Nutrition (PPN) is the delivery of nutrients via a peripheral vein.
Why is TPN bad?
Unfortunately, it can cause potentially fatal complications. TPN infusion results in impairment of gut mucosal integrity, enhanced inflammation, increased cytokine expression and trans-mucosal bacterial permeation.
Who should not receive TPN?
According to Maudar (2017), TPN is generally contraindicated in the following conditions: Infants with less than 8 cm of the small bowel. Irreversibly decerebrate patients. Patients with critical cardiovascular instability or metabolic instabilities.
Does TPN give you energy?
TPN is beneficial because it provides nutrients that are vital in maintaining high energy, hydration and strength levels. Also, it will allow patients to heal more quickly and feel more energized.
What can cause hypoglycemia in non diabetics?
- Drinking too much alcohol. When a person’s blood sugar levels are low, the pancreas releases a hormone called glucagon. …
- Medication. …
- Anorexia. …
- Hepatitis. …
- Adrenal or pituitary gland disorders. …
- Kidney problems. …
- Pancreatic tumor.
What happens if too much glucose is administered during hypoglycemia?
Rapid or excessive administration can induce hyperosmolar syndrome, and prolonged use (especially when insulin levels are high) can lead to hypokalemia. After D50W treatment, IV dextrose 5% or 10% in water is used to maintain BG levels >100 mg/dL.
What level of blood glucose is hyperglycemia?
Hyperglycemia doesn’t cause symptoms until glucose values are significantly elevated — usually above 180 to 200 milligrams per deciliter (mg/dL), or 10 to 11.1 millimoles per liter (mmol/L).