Does 97012 need a modifier

Sophia Edwards
Published Mar 24, 2026
Whether it’s 97012 or 97140, by appending the 59 modifier, you will ensure that you receive reimbursement for both services.
Is CPT 97012 a timed code?
Click here to read our articles about timing therapy notes for Medicare patients. Certain CPT codes are considered ‘timed’. … Regardless of whether you spend 10, 20, or 30 minutes assisting a patient with mechanical traction (CPT 97012), you can only bill 1 unit.
Can CPT code 97140 and 97012 be billed together?
True Blue. when I looked these up I get: 97012 is a manual traction code and 97140 is a manual therapy code. They consider these to be two modalities that are not possible for the same area in the same session. That is the mutually exclusive part.
Does Medicare pay for 97012?
Services that do not meet the requirements for covered therapy services in Medicare manuals are not payable using codes and descriptions as therapy services. To be considered reasonable and necessary, the services must meet Medicare guidelines. …Can a chiropractor use GP modifier?
In late 2019, UnitedHealthCare (Optum and UHC affiliates) required a particular modifier be appended to all physical medicine services. … GP is the most appropriate for chiropractic claims, as it aligns with the therapy provider “physical therapy”.
What does CPT code 97012 mean?
From a CPT® coding perspective, 97012 is a physical medicine mechanical traction modality that does not require attendance.
Does 97140 need a modifier?
The 97140 CPT code is appended with the modifier -59 or the appropriate -X modifier.
What is the GP modifier used for?
The GP modifier indicates that a physical therapist’s services have been provided. It’s commonly used in inpatient and outpatient multidisciplinary settings. It’s also used for functional limitation reporting (FLR), as physical therapists must report G-codes, severity modifiers, and therapy modifiers.What modifier is used for 97124?
When billed on the same visit as a chiropractic manipulative treatment code (98940-98943), carriers often require the -59 (or XS) modifier appended to the 97124 code to clarify that it’s a distinct and separate procedure being performed in a body region different from the adjustment.
Does CPT code 97010 need a modifier?This policy change requires that claims with physical medicine services 97010-97799 will require modifier GP. The modifier is required for dates of service after April 1, 2021. Any PT now billed to Anthem will require the GP modifier.
Article first time published onHow do you bill mechanical traction?
Description for CPT code 97012 Traction is generally used for joints, especially of the lumbar or cervical spine, with the expectation of relieving pain in or originating from those areas, or increasing the range of motion of the joint.
What is the difference between 97140 and 97124?
97124 is for increasing circulation and to promote tissue relaxation to the muscles. … 97140 is used to describe therapy which increases active pain-free range of motion, increased extensibility of myofascial tissue and facilitates return to functional activities. This code is reported in units of 15 minutes.
What is the CPT code for manual therapy?
Reporting Manual Therapy Services Physical and occupational therapists typically report CPT code 97140 for services best described as manual therapy techniques.
What modifiers are used for chiropractic billing?
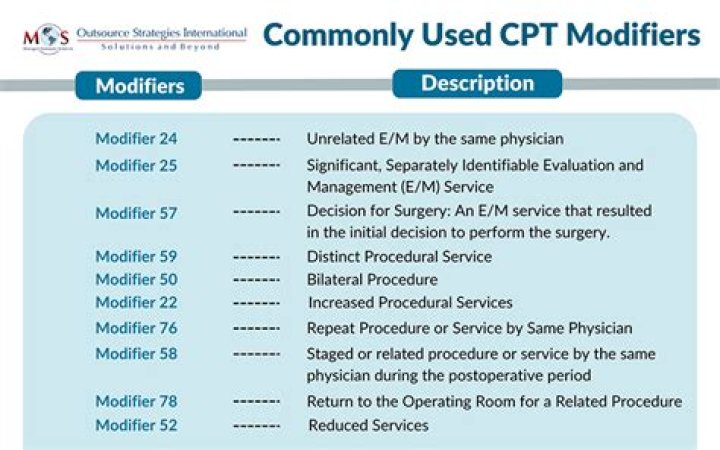
Chiropractic modifiers can be attached to certain CPT codes to tell insurance companies that there is something different about the services related to the CPT code being billed. While there are several modifiers, the two most commonly used in modifiers by chiropractors are modifier 25 and modifier 59.
What CPT codes can chiropractors use?
- 98940 Chiropractic Manipulative Treatment (CMT) …
- 98941 Chiropractic Manipulative Treatment (CMT) …
- 98942 Chiropractic Manipulative Treatment (CMT) …
- 98943 Chiropractic Manipulative Treatment (CMT)
Can a chiropractor bill CPT 97110?
Here is a list of the other most commonly used CPT codes for chiropractors, which include other treatments and appointment types: CPT Code 99202 – Evaluation and Management, Initial Visit. CPT Code 99203 – Evaluation and Management, Initial Visit. … CPT Code 97110 – Therapeutic Exercise.
What is the CPT code 97140?
97140 CPT Code Description: Manual therapy techniques (e.g., mobilization/manipulation, manual lymphatic drainage, manual traction), 1 or more regions, each 15 minutes.
When should modifier 22 be used?
Modifier 22 is used for increased procedural services and demonstrates when a physician has gone above and beyond the typical framework of a particular procedure.
Is 97140 a chiro code?
Per CPT® guidelines, 97140 describes manual therapy techniques, such as mobilization and manipulation, manual lymphatic drainage, and manual traction. Chiropractic adjustments have their own set of codes (98940-98942, or 98943 for an extremity).
Does Medicare pay for mechanical traction?
It’s covered as durable medical equipment (DME). An agreement by your doctor, provider, or supplier to be paid directly by Medicare, to accept the payment amount Medicare approves for the service, and not to bill you for any more than the Medicare deductible and coinsurance.
What is the CPT code for mechanical traction?
What is CPT Code 97012 (Traction/Mechanical Modality)? Traction is generally used for joints, especially of the lumbar or cervical spine, with the expectation of relieving pain in or originating from those areas, or increasing the range of motion of the joint.
What is mechanical traction?
Traction is a form of decompression therapy that we are happy to offer at Physical Therapy Services. It relieves pressure on the spine and alleviates pain from joints, sprains, and spasms.
Can CPT code 97124 and 97140 be billed together?
If the care you provide meets the appropriate criteria, you can add modifier 59 to indicate it was a separate service and should be payable in addition to the 97140. It’s important to note that you can never bill 96523 or 97124 with 97140, because these codes represent mutually exclusive procedures.
Is 97124 a physical therapy Code?
97124 CPT Code: Massage Therapy 97124 CPT Code Description: Therapeutic procedure, 1 or more areas, each 15 minutes; massage, including effleurage, petrissage, and/or tapotement (stroking, compression, percussion). Massage is classified as a therapeutic procedure which is a time-based service.
Does G0283 need modifier?
Medicare does need the modifier GP appended to G0283, just like the other therapy chgs require mod GP. If there is no GP, it should be denied.
Does 97026 need a modifier?
For instance, you can code 97026 GP. Most often for acupuncture, only the one modifier is needed but if you ever receive a denial for a therapy being inclusive to another service billed the same date you also want to use modifier 59 to designate that the services were separate and distinct.
What is the co modifier?
•CO modifier: Outpatient occupational therapy services furnished in whole or in part by an occupational. therapy assistant.
Which modifier goes first 59 or GP?
Always add 26 before any other modifier. If you have two payment modifiers, a common one is 51 and 59, enter 59 in the first position.
Is 97010 a billable code?
CPT Code 97010 is a misunderstood Medicare billing code. It’s often overbilled throughout healthcare because it is difficult to establish appropriate rationale to prove medical necessity for this to be separately billed in the office. … In this instance, it means 97010 is not a separately payable Medicare billing code.
Is 97012 a physical therapy Code?
CPT® 97012, Under Supervised Physical Medicine and Rehabilitation Modalities. The Current Procedural Terminology (CPT®) code 97012 as maintained by American Medical Association, is a medical procedural code under the range – Supervised Physical Medicine and Rehabilitation Modalities.
What is the CPT code for therapeutic exercise?
CPT 97110: Therapeutic Procedure CPT code 97110 is defined as “therapeutic exercises to develop strength, endurance, range of motion and flexibility.” It applies to a single or multiple body parts, and requires direct contact with a qualified healthcare professional.